
Bone health myths often mislead people about what truly strengthens bones. Strong bones require more than just calcium; factors like vitamin D, weight bearing exercise, hormonal balance, and proper diagnosis play crucial roles in building and maintaining bone strength. Hormone balance also matters, and since bone loss is often silent, early screening helps prevent fractures.
Key takeaways
- Osteoporosis and low bone density can affect men, younger adults, and even teens, not only older women.
- Peak bone mass is usually reached by about age 30 after that, bone loss speeds up with inactivity, poor diet, smoking, heavy alcohol, or certain diseases.
- Calcium supports bone structure, but vitamin D (plus magnesium and vitamin K) is needed to absorb and lock minerals into bone.
- Weight bearing and resistance exercise (walking, stairs, lifting, bands) signals bones to rebuild stronger and also improves balance to prevent falls.
- Bone thinning is often symptom free until a fracture, so screening and risk factor review matter.
- Lifestyle upgrades and modern treatments can slow loss, improve density, and sharply cut fracture risk.
Why bone health is important

Bone health matters because your bones do much more than hold you up. They support your body’s structure, protect vital organs, store essential minerals like calcium and phosphorus, and work with muscles to help you move smoothly. Strong bones also keep your posture stable and your balance steady, which is key for staying active and independent as you age.
When bones weaken, the risk of fractures rises even from small falls or minor bumps. These fractures, especially in the hip, spine, and wrist, can cause long term pain, reduced mobility, and loss of confidence in daily activities. Because osteoporosis often develops silently without clear symptoms, building and protecting bone strength early is one of the best ways to prevent future disability and maintain quality of life.
Bone Health Myths Busted
It’s easy to pick up bone health advice from family, social media, or old beliefs. But many popular ideas are incomplete or outdated. Clearing up these myths helps you focus on what truly protects bone density and prevents fractures.
Myth 1: Bone loss after menopause or aging is unavoidable.
Fact: Menopause and aging do speed bone loss, but they don’t make osteoporosis inevitable. Bone is living tissue that responds to the signals you give it, especially mechanical loading. Regular resistance training and weight bearing activity slow bone breakdown and can preserve or modestly improve bone mineral density (BMD), particularly in the hip and spine. Good nutrition supports this process, and if risk is high, medications can greatly reduce future fractures. The direction of bone loss is changeable, and starting early gives the best payoff.
Myth 2: If there’s no pain, bones must be fine.
Fact: Osteoporosis is famously a “silent disease.” Most people don’t notice any symptoms while bone density declines, and pain typically shows up only after a fracture or spinal compression. That’s why relying on how you feel is unreliable. DEXA scans and routine risk checks are the safe way to detect hidden bone loss early, especially after menopause, after age 50, or if you’ve had a low impact fracture. Waiting for pain often means waiting until damage is already done.
Myth 3: Only older women get osteoporosis.
Fact: Osteoporosis is common in postmenopausal women, but bone loss can begin earlier, and men can develop it too. Risk increases with low body weight, smoking, heavy alcohol use, long term steroid therapy, and conditions like diabetes, rheumatoid arthritis, thyroid/parathyroid disorders, or malabsorption diseases. In men, low testosterone also contributes to weaker bones. So osteoporosis isn’t a “grandmother only” issue it’s a lifelong bone strength issue for everyone.
Myth 4: Calcium supplements alone prevent fractures.
Fact: Calcium is essential, but pills by themselves don’t guarantee stronger bones. Bone strength depends on absorption (vitamin D helps), use (exercise drives minerals into bone), and overall diet quality. Research shows calcium or vitamin D supplements alone don’t reliably prevent fractures for most adults unless there is a deficiency or a broader osteoporosis plan. Think of calcium as one building block still useless without the rest of the construction team.
Myth 5: Walking is enough to build strong bones.
Fact: Walking is great for heart health and helps slow bone loss, but it provides limited stimulus for building new bone in high risk areas like hips and spine. Resistance training creates stronger, targeted loads that bones adapt to by becoming denser. The most effective routine combines frequent weight bearing activity (walking, stairs, dancing) with progressive strength training 2–3 times per week.
Myth 6: Exercise is risky if you already have osteoporosis.
Fact: The bigger risk is not exercising. Safe, guided strength and balance training improves muscle, posture, coordination, and often BMD, which lowers fracture risk. Programs should avoid extreme twisting or deep forward bending of the spine in severe osteoporosis, but still include effective moves like squats, hip hinges, step ups, rows, and balance work. Exercise is part of treatment, not something to fear.
Myth 7: Thin people have healthier bones.
Fact: Very low BMI is a well known risk factor for osteoporosis. Less body weight means less mechanical loading on bone, and low muscle/fat mass can reduce protective hormones like estrogen. Healthy weight and muscle support bone remodeling and help prevent falls. Being “too thin” is not protective for bones.
Myth 8: Caffeine always weakens bones.
Fact: The caffeine–bone link depends on dose and calcium intake. Moderate coffee or tea isn’t clearly harmful for most people, and some newer research even finds neutral or slightly protective associations when intake is moderate. The main concern is very high caffeine, which can slightly increase calcium loss and may speed bone loss in people who already consume too little calcium. Simple fixes help: keep caffeine moderate and pair it with adequate calcium (for example, dairy or fortified milk alongside coffee).
Myth 9: Alcohol doesn’t affect bone much.
Fact: Alcohol has a dose response effect on bones. Heavy drinking lowers bone formation, disrupts vitamin D and calcium handling, and weakens muscle and balance, so falls and fractures become more likely. Studies consistently link long term heavy intake with lower BMD and higher fracture risk. Light or occasional drinking seems less harmful, but protecting bones means avoiding regular heavy use and prioritizing nutrition and exercise.
Myth 10: A fracture after 50 is just bad luck.
Fact: A low impact fracture after midlife is often a fragility fracture, a warning sign of hidden osteoporosis. These fractures commonly occur from a fall at standing height or less, and they strongly predict future fractures. Guidelines recommend that any such fracture after age 50 should trigger bone health evaluation, DEXA screening, and a prevention or treatment plan to stop the repeat fracture cycle.
What Really Builds Strong Bones

Strong bones are not created by one “super nutrient” or a single workout. They are built through steady bone remodeling over years, which needs two things: enough nutrients to form bone, and regular physical loading to signal bones to stay dense. The best results come from combining nutrition, targeted exercise, and lifestyle habits, plus screening and treatment when risk is high.
- Calcium and vitamin D: Calcium is the main mineral in bone, and vitamin D helps your body absorb and use it well. Aim to meet needs through foods like dairy, fortified plant milks, calcium set tofu, sardines or salmon with bones, leafy greens, beans, almonds, and sesame, and add supplements only if diet or sunlight is not enough
- Protein and key micronutrients: Protein builds the bone framework and protects muscle, while magnesium, vitamin K, zinc, and overall calorie intake support mineralization and bone strength. Long term low protein or under eating speeds bone loss.
- Progressive resistance training: Strength training 2–3 times weekly is one of the strongest drivers of hip and spine density. Examples include squats, lunges, step ups, hip hinges, rows, presses, and resistance bands.
- Regular weight bearing or impact movement: Activities that work against gravity help maintain density and slow age related loss. Do brisk walking, stair climbing, dancing, hiking, or light jogging most days if joints allow.
- Balance and fall prevention: Since most fractures happen after falls, balance training is essential. Tai chi, yoga, single leg stands, and core/hip stability drills reduce fall risk and protect independence.
- Bone friendly lifestyle habits: Avoid smoking, limit heavy alcohol, keep caffeine moderate, maintain a healthy stable weight, stay active, and sleep 7-9 hours to support healthy remodeling.
- Screening and treatment when needed: Because bone loss is silent, DEXA screening at the right time catches risk early. If osteoporosis or high fracture risk is found, medications can greatly reduce future fractures alongside lifestyle care.
Bone Health at Different Ages
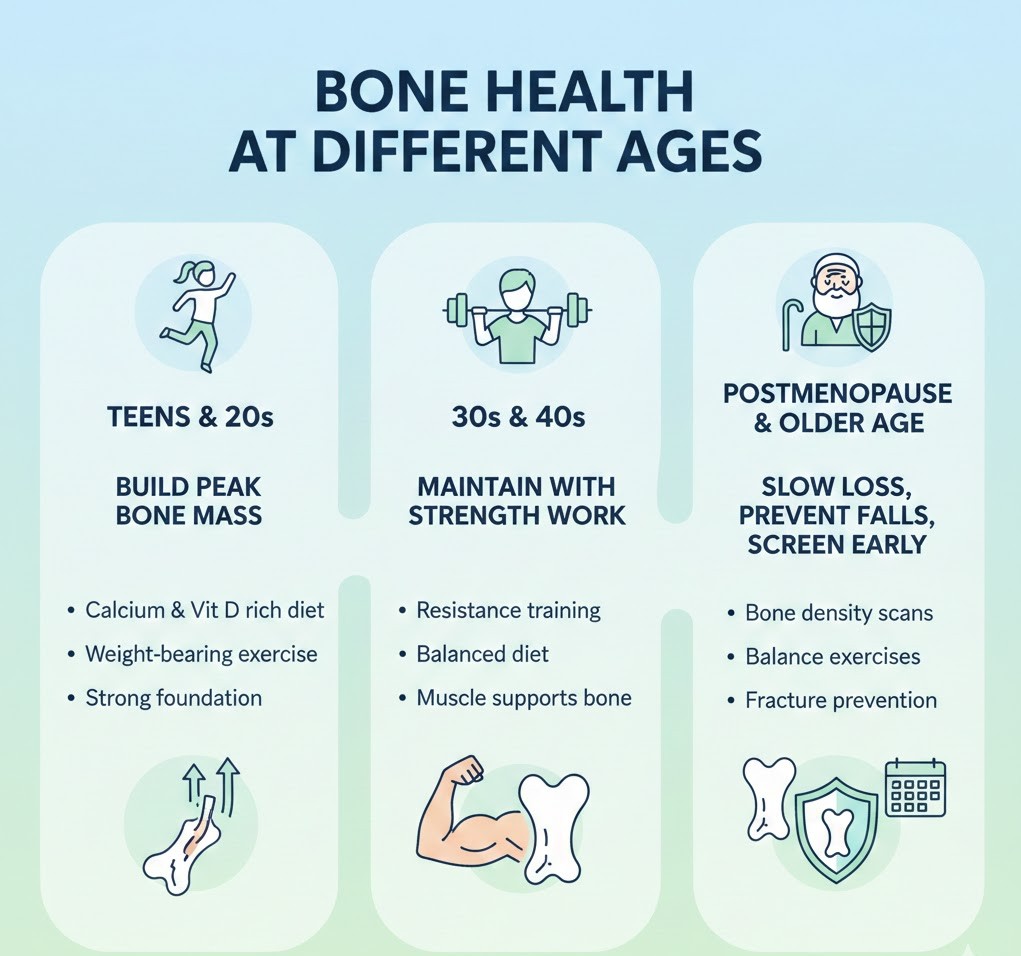
Bone needs change across life because your body builds bone early, maintains it in midlife, and gradually loses it later. Building a strong “bone bank” when you’re young makes it easier to prevent osteoporosis and fractures as you age.
- Teens and 20s (build peak bone mass): This is the main bone building stage. Good nutrition, enough vitamin D, and regular impact or sports activity help you reach higher peak bone strength for life.
- 30s and 40s (maintain with strength work): Bone starts declining slowly, so resistance training and steady calcium, vitamin D, and protein intake help protect hip and spine density.
- Postmenopause and older age (slow loss, prevent falls, screen early): Estrogen drop speeds bone loss, so strength and balance training plus early DEXA screening are key to preventing silent thinning and fragility fractures.
Hidden Risk Factors People Miss
Some risks don’t look obvious day to day, so people ignore them until bone loss is advanced. If you have any of these, earlier screening and prevention are smart.
- Long term steroid use: Medicines like prednisone for asthma, arthritis, or autoimmune disease speed bone breakdown and weaken bone structure over time.
- Thyroid or parathyroid disorders: These hormone problems can disturb calcium control in the body and accelerate bone loss.
- Low vitamin D or malabsorption: Conditions like celiac disease, gut disorders, or bariatric surgery reduce calcium absorption and lower bone density.
- Chronic illnesses: Diabetes and rheumatoid arthritis increase osteoporosis risk through inflammation and medication effects.
- Past fragility fracture after 50: A low impact fracture after midlife is a strong warning sign and predicts higher future fracture risk, even if you feel fine now.
DEXA Screening: When and Why
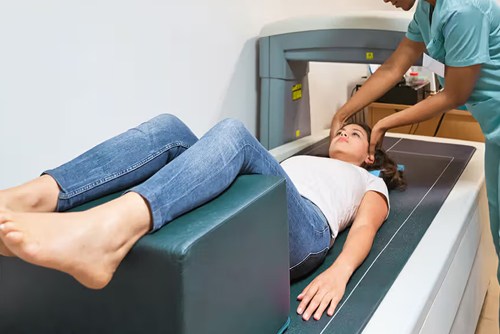
Bone loss usually happens without symptoms, so a DEXA scan is the most reliable way to check bone strength before fractures occur. It measures bone mineral density in the hip and spine, classifies risk as normal, osteopenia, or osteoporosis, and helps guide prevention or treatment early.
Who needs it?
- Women 65+ because osteoporosis risk rises sharply and is often silent.
- Postmenopausal women under 65 with risk factors like early menopause, family history, low BMI, smoking, steroids, inactivity, heavy alcohol, or bone affecting illnesses.
- Anyone over 50 with a low impact fracture since this often signals fragile bones and high repeat fracture risk.
Quick Bone Strength Routine
Bones get stronger with regular loading, not occasional effort. A weekly mix of strength, weight bearing movement, balance work, and recovery habits keeps bones dense, muscles supportive, and fall risk low.
- Strength training (2-3 days/week): Full body resistance focusing on hips and spine (squats or sit to stands, stepups, hip hinges, rows, presses), with gradual progress in load.
- Weight-bearing activity (most days): 30-45 minutes of brisk walking, stairs, dancing, or hiking to keep bones responsive to gravity.
- Balance work (daily 5-10 minutes): Single leg stands, heel to toe walking, tai chi, or yoga to prevent falls.
- Protein daily: Include protein at each meal to support bone matrix and muscle strength.
- Calcium and vitamin D support: Eat calcium rich foods every day and ensure enough vitamin D through safe sun or supplements if needed.
- Bone friendly habits: Don’t smoke, limit heavy alcohol, maintain a healthy stable weight, and sleep well to slow bone breakdown.
Conclusion
Bone health myths often mislead people into thinking calcium alone strengthens bones, but true bone strength depends on a combination of factors including vitamin D, magnesium, vitamin K, weight bearing and resistance exercise, hormonal balance, and early screening to detect silent bone loss. Osteoporosis can affect not just older women but men, younger adults, and teens, and bone loss accelerates with inactivity, poor diet, smoking, and alcohol. Exercise, especially resistance training and weight bearing activity stimulates bone remodeling and density, while balance training helps prevent falls that cause fractures. Calcium supports bone structure but requires vitamin D for absorption and is only effective alongside proper nutrition, exercise, and lifestyle habits. Since bone thinning is often symptomless until fractures occur, regular DEXA screening is key for early diagnosis and timely treatment to slow bone loss and reduce fracture risk.
FAQs
Is calcium enough to build strong bones?
No. Calcium is essential, but bones also need vitamin D to absorb calcium, plus protein and other nutrients like magnesium and vitamin K. Without exercise and healthy habits, calcium alone can’t fully protect bone density.
Who can get osteoporosis besides older women?
Anyone. Men, younger adults, and even teens can develop low bone density, especially with risk factors like low BMI, smoking, heavy alcohol use, steroid medicines, or certain medical conditions.
When do we reach peak bone mass?
Peak bone mass is usually reached around age 30. After that, bone loss slowly begins and speeds up with inactivity, poor nutrition, smoking, heavy alcohol use, and some illnesses.
If I don’t have bone pain, does that mean my bones are healthy?
Not necessarily. Osteoporosis is often a silent disease. Many people feel nothing until a fracture occurs, which is why screening is important.
What type of exercise builds bone best?
Progressive resistance training (weights, bands, bodyweight strength) is most effective for hips and spine. Weight bearing movement like walking or stairs supports maintenance, and balance training prevents falls.
Is walking enough for bone strength?
Walking helps slow bone loss, but it’s not the strongest bone builder. Adding resistance training 2-3 times per week makes a bigger difference for bone density.
Is exercise unsafe if I already have osteoporosis?
No. Safe, guided strength and balance training is one of the best treatments. It improves muscle, posture, coordination, and reduces fall and fracture risk.
Does being thin protect you from osteoporosis?
Actually, very low BMI increases risk. Healthy weight and muscle provide mechanical load and hormonal support that help protect bones.
Do caffeine and coffee weaken bones?
Moderate caffeine is usually fine if calcium intake is adequate. Very high caffeine with low calcium may slightly raise bone loss risk, so moderation matters more than avoidance.
How much alcohol is harmful for bones?
Heavy or frequent drinking harms bones by reducing bone formation and increasing fall risk. Light to moderate intake is less risky, but “more is better” is not true for bone health.
When should someone get a DEXA scan?
Women should screen at 65, earlier if postmenopausal with risk factors. Anyone over 50 with a low impact fracture should also be evaluated.
Can bone loss be reversed?
Significant loss is hard to fully reverse, but it can be slowed or partly improved. Strength training, good nutrition, and medications (if needed) reduce fracture risk and often improve bone density over time.
References
- Bone Myths & Truths. (2013, January 12). Bumrungrad International Hospital. Retrieved November 26, 2025, from https://www.bumrungrad.com/en/health-blog/stay-active-pain-free/bone-myths-truths
- Carteron, N. (2017, December 8). Osteoporosis Myths and Bone Health Facts. Healthline. Retrieved November 26, 2025, from https://www.healthline.com/health/osteoporosis-myths#not-natural-aging
- Nicole Shue. (2023, May 30). 5 Myths About Osteoporosis. Kieser Australia. Retrieved November 26, 2025, from https://www.kieser.com.au/blog/posts/5-myths-about-osteoporosis
- Pitone, M. L. (n.d.). 3 Ways to Build Strong Bones | Nemours KidsHealth. Kids Health. Retrieved November 26, 2025, from https://kidshealth.org/en/parents/strong-bones.html
- Vichare, P. (2025, April 20). Top 10 Bone and Joint Health Myths Debunked. ANSSI Wellness. Retrieved November 26, 2025, from https://www.anssiwellness.com/orthopaedic-myths-vs-facts-debunking-common-misconceptions-about-bone-and-joint-care/
Aubrey Carson is an RDN with 9 years across hospital, outpatient, and private practice settings. They earned an MS in Clinical Nutrition from Tufts University – Friedman School (2016) and completed a Dietetic Internship at Mayo Clinic. Aubrey specializes in micronutrient assessment, evidence-based supplementation, and patient education. Their work includes CE presentations for the Academy of Nutrition and Dietetics and collaborations with Mass General Brigham on nutrition education resources.

