Bone health is essential for strength, balance, and overall mobility. However, many people don’t realize that chronic diseases can silently damage their bones over time. Conditions such as diabetes, thyroid disorders, kidney disease, and arthritis interfere with the body’s natural bone renewal process, making bones thinner, weaker, and more prone to fractures. Understanding how Chronic Disease Weaken Your Bone is the first step toward preventing complications and maintaining lifelong skeletal health.
Key Takeaways
- Chronic illnesses disrupt bone formation, calcium absorption, and hormone balance, weakening bone structure over time.
- Common diseases that affect bones include diabetes, thyroid disorders, kidney disease, rheumatoid arthritis, and digestive disorders.
- Certain long-term medications may accelerate bone loss.
- Balanced nutrition, physical activity, and early medical management can help protect bone health.
- Regular bone density testing is essential for people with chronic conditions.
What Are Chronic Diseases?
Chronic diseases are long-term health conditions that develop slowly and persist for months or even years. Unlike short-term illnesses, they often require ongoing medical care and lifestyle management. Common examples include diabetes, heart disease, kidney disease, arthritis, thyroid disorders, and hypertension.
These conditions can affect various systems of the body, including the bones, by disrupting hormone levels, nutrient absorption, or blood circulation. Over time, the stress of managing a chronic illness and certain medications used to treat it can contribute to bone loss and reduced bone strength. Understanding how these diseases influence bone health is key to preventing long-term complications.
The Connection Between Chronic Diseases and Bones
Chronic diseases and bone health are closely linked. Many long-term illnesses disrupt the body’s ability to absorb nutrients, regulate hormones, and rebuild bone tissue effectively. Over time, this leads to reduced bone mineral density, making bones fragile and more likely to break. Inflammation, poor circulation, and limited physical activity are common effects of chronic diseases that also contribute to gradual bone loss.
When chronic conditions go unmanaged, they create a cycle where weakened bones increase vulnerability to injury, further limiting movement and overall health. Recognizing this connection helps in taking early steps to preserve bone strength and prevent fractures.
How Chronic Disease Weaken Your Bone
Bones are constantly renewing themselves through a process called remodeling, where old bone tissue is replaced by new. Chronic illnesses interfere with this process by disrupting calcium absorption, hormone balance, or blood supply to bone tissue. For example, diabetes affects bone formation through high blood sugar and insulin resistance, while kidney disease alters calcium and vitamin D balance.
Some chronic conditions also increase inflammation, which activates bone destroying cells and slows the body’s ability to rebuild strong bone tissue. In addition, medications used to manage long-term diseases like corticosteroids or thyroid treatments can further weaken bones when used for extended period
Common Chronic Diseases That Weaken Bones
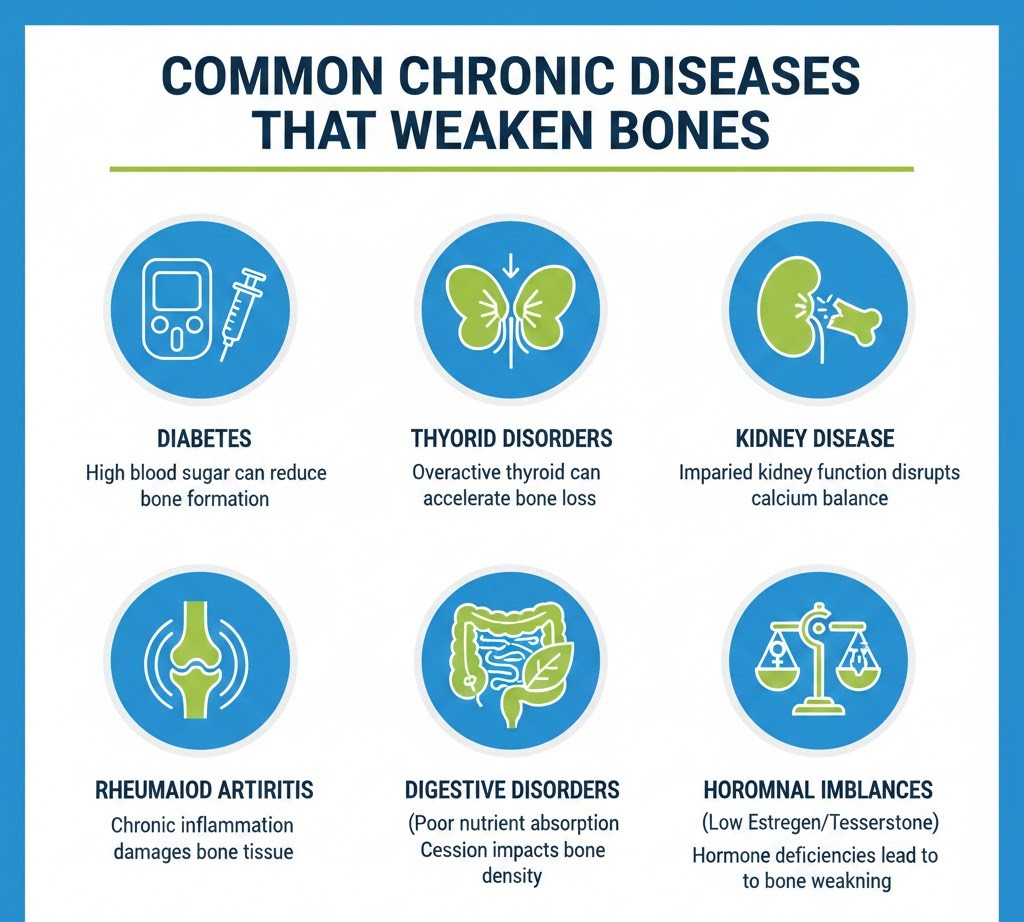
Several chronic diseases can gradually weaken bones by affecting hormone balance, nutrient absorption, or bone cell activity. These conditions may not cause immediate symptoms but can silently reduce bone density and increase the risk of fractures over time. Understanding how each disease impacts bone health is essential for effective prevention and management.
1. Diabetes
Both Type 1 and Type 2 diabetes negatively impact bone health and healing. High blood sugar levels and insulin resistance disrupt the bone remodeling process, leading to weaker, more fragile bones. Poor circulation and nerve damage further increase the risk of fractures and slow recovery after injury. Over time, uncontrolled diabetes can significantly reduce bone quality and density. Proper glucose control and weight-bearing exercise are key to minimizing these effects.
2. Thyroid Disorders
The thyroid gland plays a major role in regulating bone metabolism. Excess thyroid hormones, as seen in hyperthyroidism, cause rapid bone turnover and lead to bone thinning. Conversely, hypothyroidism slows bone renewal and affects calcium regulation, resulting in weaker bones. Long-term imbalance in thyroid hormones can raise the risk of osteoporosis. Regular thyroid function testing and medication management are essential for bone preservation.
3. Kidney Disease
Healthy kidneys regulate calcium, phosphorus, and vitamin D minerals essential for bone strength. In chronic kidney disease (CKD), these regulatory functions decline, causing an imbalance that leads to brittle, fragile bones. This condition, known as renal osteodystrophy, makes fractures more likely even from minor injuries. Poor kidney function also limits vitamin D activation, weakening bone mineralization. Early kidney care and nutritional support can reduce bone complications.
4. Rheumatoid Arthritis
Rheumatoid arthritis causes chronic inflammation that damages joints and nearby bones over time. Inflammatory chemicals break down bone tissue, while long-term corticosteroid use further accelerates bone loss. The combination of inflammation and medication side effects significantly increases fracture risk. Reduced mobility from joint pain also contributes to weaker bones. Managing inflammation and maintaining physical activity are vital for bone strength.
5. Digestive Disorders
Conditions such as Crohn’s disease, celiac disease, and ulcerative colitis interfere with nutrient absorption, especially calcium and vitamin D. Without these nutrients, bones become porous, thin, and prone to fractures. Chronic digestive inflammation can also disrupt hormonal signals that regulate bone growth. People with these disorders often develop osteoporosis earlier than others. A nutrient-rich diet and medical management help protect bone health.
6. Hormonal Imbalances
Hormones such as testosterone and estrogen are essential for bone renewal. Low testosterone in men and low estrogen in women slow bone formation and increase bone fragility. Disorders of the adrenal or parathyroid glands can also alter calcium and hormone levels, leading to bone loss. These imbalances make bones thinner and weaker over time. Hormone testing and targeted treatment help restore bone strength and prevent fractures.
Medications That May Affect Bone Strength
Long-term use of certain medications prescribed for chronic diseases can unintentionally weaken bones by disrupting calcium absorption or slowing bone formation. It’s important to understand these risks and take preventive measures if you rely on such treatments.
Common medications that may impact bone health include:
- Corticosteroids: Used for asthma, arthritis, and autoimmune disorders; they can slow new bone formation and increase bone loss.
- Thyroid Hormone Replacements: Excess doses may speed up bone turnover, leading to bone thinning.
- Anticonvulsants: Medications for epilepsy or nerve pain can interfere with vitamin D metabolism and calcium absorption.
- Proton Pump Inhibitors (PPIs): Commonly used for acid reflux, these may reduce calcium absorption over time.
- Cancer Treatments and Hormonal Therapies: Certain drugs used in chemotherapy or hormone suppression can reduce bone density.
Complications of Weak Bones Caused by Chronic Diseases
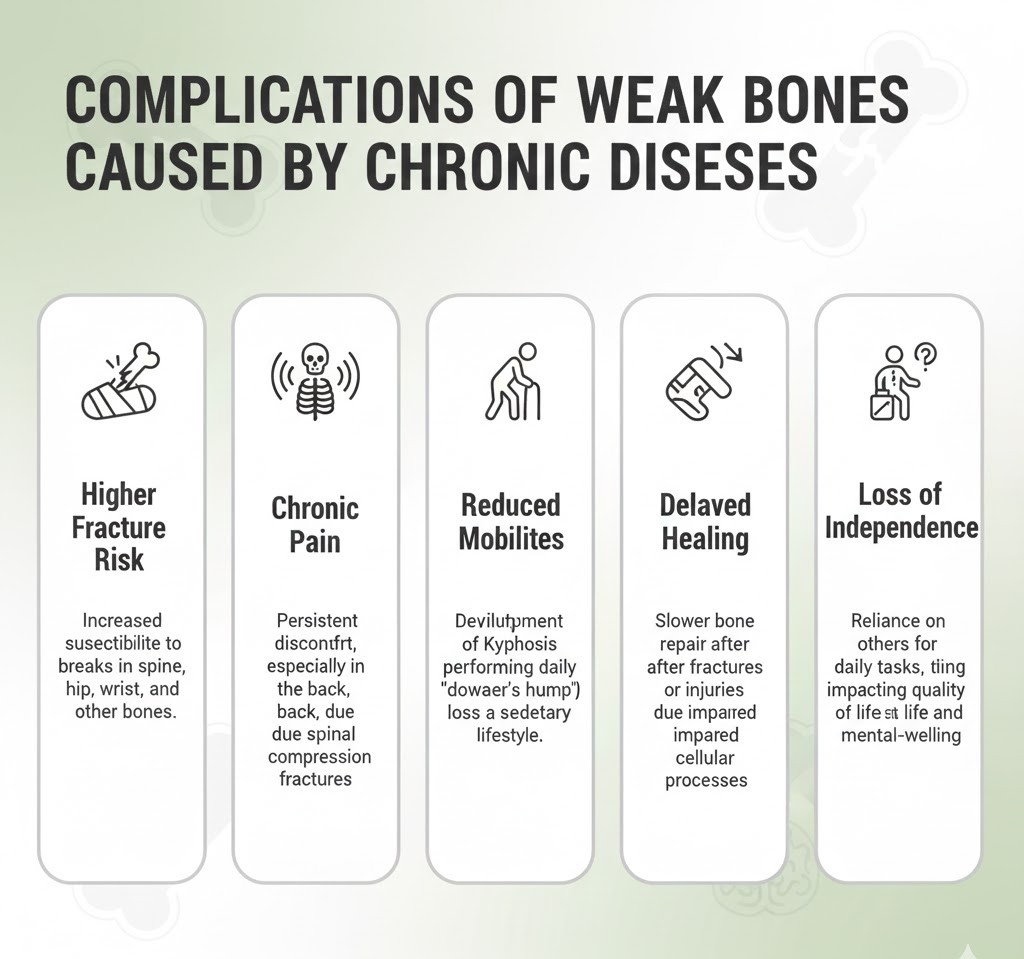
When chronic diseases weaken the bones, the effects go beyond simple discomfort. Fragile bones are more susceptible to fractures, chronic pain, and long-term mobility issues that can significantly affect quality of life. These complications can also make managing existing health conditions more challenging, highlighting the importance of early prevention and care.
Common complications include:
- Higher Fracture Risk: Fragile bones are more likely to break from minor falls or even everyday movements.
- Chronic Pain: Weakened or fractured bones can cause ongoing pain, especially in the spine and hips.
- Reduced Mobility: Fractures and stiffness make it difficult to stay active, affecting independence and physical health.
- Postural Changes: Spinal bone loss can lead to height reduction or a stooped posture over time.
- Delayed Healing: Chronic diseases like diabetes or kidney disorders slow bone and tissue recovery after injuries.
- Loss of Independence: Severe bone weakness can limit the ability to perform daily tasks without assistance.
How to Protect Your Bones If You Have a Chronic Disease
Having a chronic illness doesn’t mean you can’t maintain strong, healthy bones. With consistent care, smart habits, and proper medical management, you can minimize bone loss and preserve strength throughout life. Taking small, proactive steps can make a significant difference in long-term bone health.
- Eat a Balanced Diet: Include foods rich in calcium, vitamin D, magnesium, and protein such as dairy products, leafy greens, almonds, and fish with edible bones. These nutrients support bone renewal and strength.
- Exercise Regularly: Engage in low-impact, weight-bearing activities like walking, cycling, yoga, or light resistance training. These exercises help stimulate bone growth, improve balance, and prevent falls.
- Monitor Your Condition: Keep chronic diseases under control through regular checkups, timely medication, and lifestyle adjustments. Proper disease management prevents complications that can affect bones.
- Avoid Smoking and Limit Alcohol: Both habits interfere with calcium absorption, reduce bone density, and slow the body’s ability to form new bone tissue.
- Get Regular Bone Density Tests: Routine screenings can detect bone thinning early, allowing for timely treatment and preventive care.
When to Consult Your Doctor
Even with good lifestyle habits, chronic diseases can make bones more vulnerable over time. It’s important to seek medical advice early if you notice warning signs such as:
- Frequent or unexplained back or joint pain
- Loss of height or changes in posture
- Bone fractures from minor falls or injuries
- Persistent fatigue, weakness, or stiffness
- Long-term medication use (like corticosteroids) or low hormone levels
- Difficulty with movement, balance, or performing daily activities due to stiffness or pain
A healthcare provider may recommend bone density testing, blood work, or changes to your treatment plan. Early intervention can prevent complications like osteoporosis and fractures.
Conclusion
Chronic diseases such as diabetes, thyroid disorders, kidney disease, and arthritis can silently weaken bones over time by disrupting hormone balance, calcium absorption, and bone renewal. These conditions increase the risk of fractures, chronic pain, and reduced mobility. Certain long-term medications, including corticosteroids and thyroid treatments, may further contribute to bone loss. Maintaining a healthy lifestyle with balanced nutrition, regular exercise, and proper disease management is key to protecting bone strength. Regular bone density screenings and early medical care can help detect bone thinning early, prevent complications, and support lifelong bone health and independence.
FAQs
Can chronic diseases really weaken bones?
Yes. Chronic diseases such as diabetes, thyroid disorders, kidney disease, and arthritis can interfere with hormone balance, calcium absorption, and bone renewal, gradually leading to weaker bones and higher fracture risk.
Which chronic diseases affect bone health the most?
The most common ones include diabetes, rheumatoid arthritis, chronic kidney disease, thyroid disorders, digestive diseases (like celiac or Crohn’s), and hormonal imbalances.
How do medications for chronic diseases cause bone loss?
Certain long-term medications such as corticosteroids, thyroid hormone replacements, anticonvulsants, and some cancer therapies can reduce calcium absorption or slow new bone formation.
What are early signs of weak bones?
Early warning signs include frequent back pain, loss of height, a stooped posture, brittle nails, weak grip strength, and bone fractures from minor falls.
How can I protect my bones if I have a chronic disease?
Eat calcium and vitamin D-rich foods, exercise regularly, limit smoking and alcohol, manage your condition with regular checkups, and get bone density screenings.
How often should bone density tests be done?
People with chronic conditions or on long-term medications should get a bone density (DEXA) scan every 1-2 years, or as advised by their healthcare provider.
Can bone loss from chronic diseases be reversed?
In some cases, yes early intervention through proper diet, medication, and exercise can slow or even partially restore bone density. However, prevention is more effective than reversal.
Does inflammation from chronic illness affect bones?
Absolutely. Chronic inflammation activates bone-destroying cells (osteoclasts), which speed up bone breakdown and reduce bone density over time.
Is exercise safe for people with weak bones?
Yes. Low-impact, weight-bearing exercises such as walking, light weightlifting, and yoga are safe and effective for improving bone strength and balance.
When should I consult a doctor about bone health?
Consult your doctor if you experience unexplained bone or back pain, frequent fractures, fatigue, or take medications known to affect bone health. Early diagnosis prevents serious complications.
References
- Chronic Disease and Bone Health. (2022, March 16). National Osteoporosis Foundation of South Africa. Retrieved November 12, 2025, from https://osteoporosis.org.za/chronic-disease-and-bone-health/
- The Connection Between Chronic Inflammation and Bone Loss. (n.d.). MSK Doctors. Retrieved November 12, 2025, from https://search.mskdoctors.com/doctors/ella-mcaleese/articles/the-connection-between-chronic-inflammation-and-bone-loss
- Mulcahey, M. K. (n.d.). Impact of Chronic Illness on Bone Health – OrthoInfo – AAOS. Retrieved November 12, 2025, from https://orthoinfo.aaos.org/en/staying-healthy/impact-of-chronic-illness-on-bone-health/
Aubrey Carson is an RDN with 9 years across hospital, outpatient, and private practice settings. They earned an MS in Clinical Nutrition from Tufts University – Friedman School (2016) and completed a Dietetic Internship at Mayo Clinic. Aubrey specializes in micronutrient assessment, evidence-based supplementation, and patient education. Their work includes CE presentations for the Academy of Nutrition and Dietetics and collaborations with Mass General Brigham on nutrition education resources.

