
Diabetes is a long-term condition where the body cannot produce or effectively use insulin, leading to high blood sugar. It affects multiple organs and requires early detection, lifestyle management, medication, and regular monitoring to prevent serious complications. For a deeper overview of causes, risks, and treatment options, you can also read Everything About Diabetes.
Key Takeaways:
- Diabetes includes Type 1, Type 2, and Gestational forms, differing in cause and treatment.
- Early symptoms include thirst, frequent urination, fatigue, and unexplained weight loss (see detailed symptoms of Type 2 diabetes).
- Diagnosis is based on A1C ≥ 6.5%, fasting glucose, or glucose tolerance tests.
- Lifestyle management balanced diet, exercise, and weight control—is the foundation of care, supported by natural blood sugar control strategies.
- Medications, including insulin and GLP-1 or SGLT2 drugs, support blood sugar and organ protection.
- Preventive screening for eyes, kidneys, heart, and feet helps detect complications early.
- Vaccinations and follow-ups are vital for long-term control and quality of life.
What Is Diabetes?
Diabetes is a condition in which the body either does not produce enough insulin or cannot properly use the insulin it produces. Insulin helps move sugar (glucose) from your blood into your cells, where it’s used for energy.
Types of Diabetes
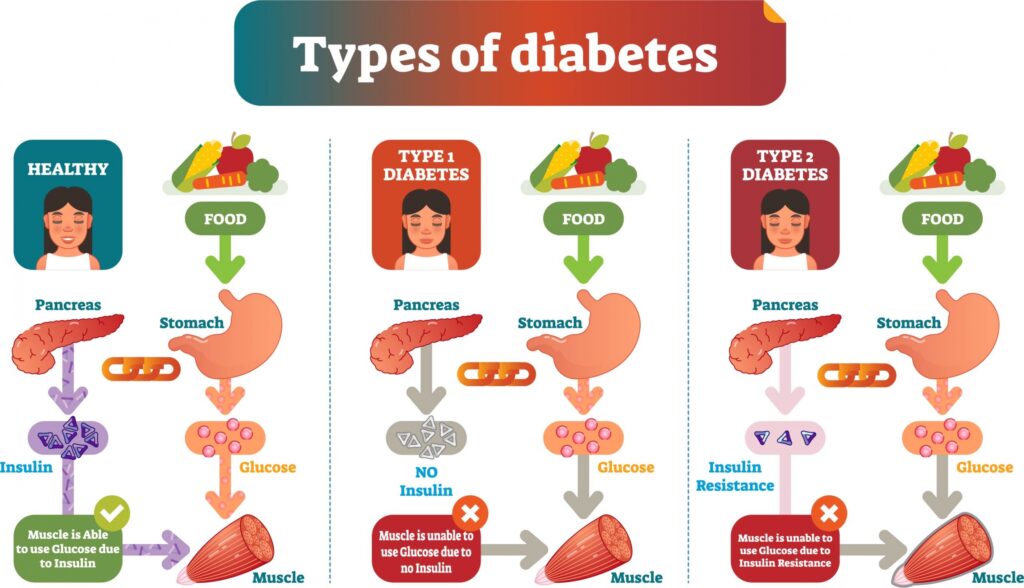
Diabetes mellitus is a chronic metabolic disorder characterized by high blood glucose levels resulting from defects in insulin secretion, insulin action, or both. It is broadly classified into several types based on the underlying cause and mechanism, the most common being Type 1 diabetes, Type 2 diabetes, and Gestational diabetes.
- Type 1 Diabetes: An autoimmune condition where the body’s immune system attacks the insulin-producing cells in the pancreas. Very little or no insulin is produced, so daily insulin injections or an insulin pump are required.
- Type 2 Diabetes: The most common type. The body becomes resistant to insulin, and the pancreas cannot produce enough over time. It often develops gradually and is strongly linked to lifestyle and genetics.
- Gestational Diabetes: Develops during pregnancy when hormones interfere with insulin use. It usually goes away after childbirth but increases the risk of type 2 diabetes later for both mother and child.
- Other Specific Types: Less common forms include monogenic diabetes (such as MODY), diabetes from pancreatic diseases like pancreatitis, or drug-induced diabetes from steroids.
For a side-by-side comparison of causes, symptoms, and treatments, see Type 1 and Type 2 diabetes.
Symptoms & When to Seek Care
Recognizing diabetes early helps prevent complications and improves outcomes.
Common Symptoms of High Blood Sugar (Hyperglycemia)
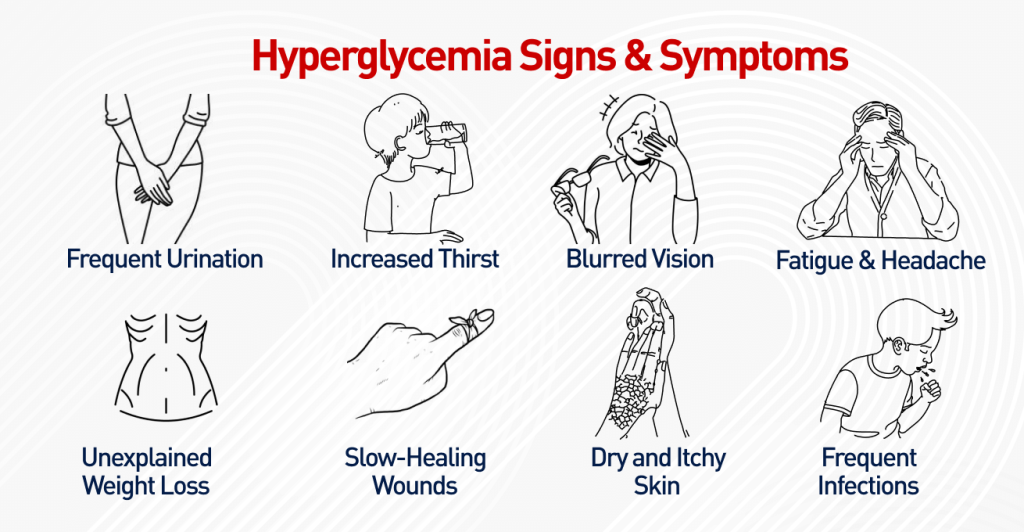
High blood sugar occurs when the body cannot effectively use or produce insulin. Common signs include:
- Increased thirst and frequent urination: Excess glucose in the blood causes the kidneys to remove more water.
- Unexplained weight loss: The body starts breaking down fat and muscle for energy due to lack of insulin.
- Fatigue or weakness: Cells don’t receive enough glucose to function properly.
- Blurred vision: High glucose levels can cause swelling in the eye lens.
- Slow-healing wounds or frequent infections: High sugar levels weaken the immune system and impair circulation.
Signs of Low Blood Sugar (Hypoglycemia)
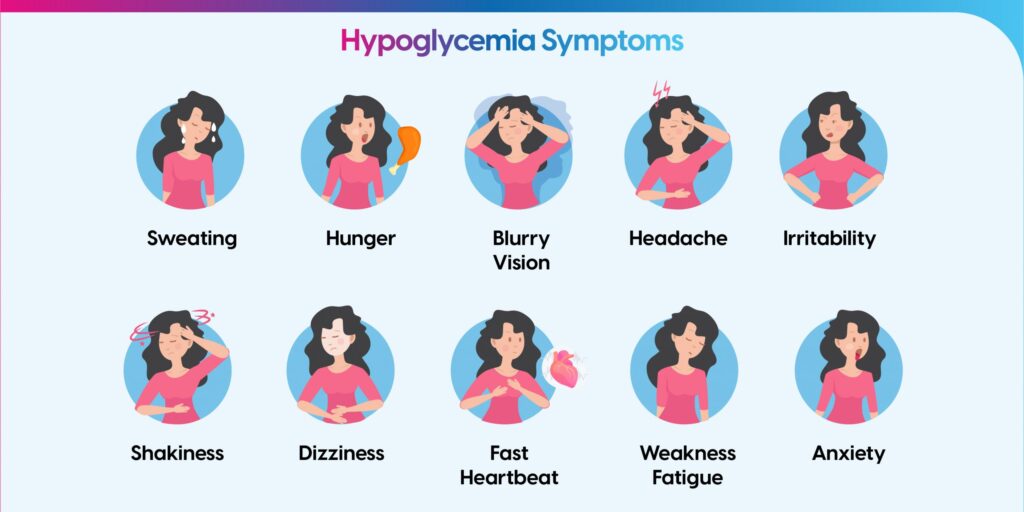
Low blood sugar, also known as hypoglycemia, happens when the level of glucose in the blood drops below normal. It most often occurs in people with diabetes who take insulin or certain oral medications that increase insulin levels.
- Trembling or sweating: The body releases adrenaline in response to low glucose, causing shakiness and perspiration.
- Hunger, irritability, or confusion: The brain depends on glucose for energy, so a drop can cause mood changes, irritability, or difficulty thinking clearly.
- Dizziness or fainting: Severe hypoglycemia can cause lightheadedness, loss of coordination, or even unconsciousness if not treated promptly.
Emergency Warning Signs
Seek immediate medical attention if you experience:
- Fast breathing or fruity-smelling breath: Could indicate diabetic ketoacidosis (a life-threatening condition).
- Confusion or drowsiness: May signal dangerously low or high blood sugar levels.
- Very high blood sugar with dehydration: Can lead to severe complications if untreated.
When to Screen Even Without Symptoms
Regular screening is important even if you feel well, especially if you:
- Are overweight or obese
- Have a family history of diabetes
- Previously had gestational diabetes during pregnancy
Early detection through routine blood tests can help manage diabetes effectively and reduce long-term health risks. If you’re unsure about timing, this guide on how often to check for diabetes can be helpful.
Diagnosis and Early Detection of Diabetes
Accurate diagnosis of diabetes is vital to ensure proper treatment, prevent complications, and promote long-term health. Early detection allows for timely management, reducing the risk of heart disease, kidney problems, nerve damage, and vision loss.
Diagnostic Tests and Thresholds
Several tests are used to measure blood glucose levels and confirm a diabetes diagnosis:
- A1C Test: Reflects the average blood sugar level over the past 2–3 months.
- Fasting Plasma Glucose (FPG): Measures blood sugar after an overnight fast of at least 8 hours.
- 2-Hour Oral Glucose Tolerance Test (OGTT): Measures blood sugar two hours after consuming a glucose drink.
- Random Plasma Glucose Test: Can be done any time of day, regardless of meals.
Prediabetes Criteria
Prediabetes is a condition where blood sugar levels are higher than normal but not yet high enough for a diabetes diagnosis. Identifying prediabetes early provides an opportunity for lifestyle changes to prevent progression to diabetes.
- A1C: Between 5.7% and 6.4%
- Fasting Plasma Glucose: Between 100–125 mg/dL
- 2-Hour OGTT: Between 140–199 mg/dL
Screening Recommendations
Regular screening helps detect diabetes and prediabetes before symptoms develop.
- Adults aged 35 years and older should be screened at least once every three years.
- Earlier or more frequent screening is advised for individuals who Are overweight or obese, Have a family history of diabetes, Had gestational diabetes during pregnancy and Have high blood pressure, high cholesterol, or a sedentary lifestyle
Differentiating Type 1 and Type 2 Diabetes
Distinguishing between Type 1 and Type 2 diabetes is important because their causes, treatment approaches, and long-term management differ.
- Type 1 Diabetes: Usually develops in younger, leaner individuals and has a rapid onset of symptoms such as excessive thirst, urination, and weight loss. It is typically caused by autoimmune destruction of the insulin-producing beta cells in the pancreas.
- Type 2 Diabetes: More common in adults, especially those who are overweight or obese, with a gradual onset of symptoms. The pancreas still produces insulin, but the body becomes resistant to its effects.
Accurate differentiation ensures appropriate treatment — insulin therapy for Type 1 and lifestyle modification, oral medications, or insulin as needed for Type 2.
Gestational Diabetes Screening
Gestational diabetes is a type of diabetes that develops during pregnancy due to hormonal changes that affect insulin function.
- When to Screen: Screening is typically performed between 24 and 28 weeks of pregnancy, when insulin resistance tends to increase.
- How It’s Done: A glucose tolerance test (GTT) is used. The expectant mother drinks a glucose solution, and blood sugar levels are measured after a set period (usually 1 or 2 hours).
Early detection and proper management help prevent complications such as high birth weight, preterm delivery, and future Type 2 diabetes in both mother and child.
Risk Factors for Diabetes
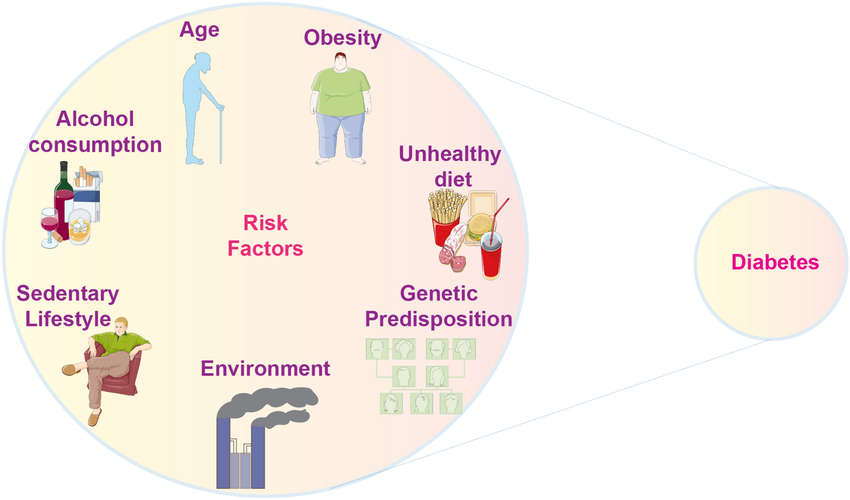
Identifying what increases your risk of developing diabetes is essential for early prevention and lifestyle modification. Some risk factors cannot be changed, while others can be managed or eliminated through healthy choices.
Non-Modifiable Factors
These are factors you cannot change, but knowing them helps guide screening and early monitoring:
- Family History: Having a parent or sibling with diabetes significantly raises your risk.
- Age: The risk increases with age, especially after 35–40 years.
- Ethnicity: People of Asian, African, Hispanic, or Indigenous descent have a higher susceptibility to diabetes.
- History of Gestational Diabetes: Women who developed diabetes during pregnancy are more likely to develop Type 2 diabetes later in life.
Modifiable Factors
These are lifestyle-related risks that can be improved or reversed through behavior changes:
- Being Overweight or Obese: Excess body fat, especially around the abdomen, increases insulin resistance.
- Lack of Physical Activity: A sedentary lifestyle lowers insulin sensitivity and contributes to weight gain.
- Unhealthy Diet: Diets high in processed foods, refined carbohydrates, and sugary drinks raise blood sugar levels. To reduce risk, knowing foods to avoid with diabetes is especially helpful.
- Smoking or Heavy Alcohol Use: Both can impair insulin function and worsen other diabetes risk factors.
- Poor Sleep or Sleep Apnea: Chronic sleep deprivation or disrupted sleep affects metabolism and insulin regulation.
Specific Risks
In addition to general risk factors, certain specific conditions or situations can further increase the likelihood of developing diabetes.
- Women with Gestational Diabetes: Have a significantly higher chance of developing Type 2 diabetes in the future.
- Certain Medications or Medical Conditions: Long-term use of steroids, some antipsychotics, or conditions such as pancreatitis can increase diabetes risk.
Early awareness and lifestyle adjustments such as maintaining a healthy weight, exercising regularly, eating balanced meals, and avoiding smoking can greatly reduce the likelihood of developing diabetes.
How Diabetes Affects the Body
Diabetes affects the body in several interconnected ways, depending on whether it’s Type 1, Type 2, or gestational diabetes. Here’s a breakdown of how it impacts different systems:
1. The Core Problem: High Blood Sugar (Hyperglycemia)
Diabetes occurs when the body doesn’t produce enough insulin (Type 1) or can’t effectively use insulin (Type 2). Insulin is the hormone that helps glucose enter cells for energy. Without proper insulin function:
- Glucose builds up in the bloodstream.
- Cells are starved of energy.
- Over time, this damages blood vessels and organs.
2. Cardiovascular System
High blood sugar damages blood vessel walls, leading to:
- Atherosclerosis (narrowing of arteries)
- Increased risk of heart attack, stroke, and high blood pressure
- Poor circulation, especially in the legs and feet
3. Nervous System (Neuropathy)
Excess glucose can damage the nerves, leading to:
- Peripheral neuropathy: tingling, burning, or numbness in hands and feet
- Autonomic neuropathy: affects internal organs—causing digestive issues, bladder problems, or erectile dysfunction
4. Eyes (Diabetic Retinopathy)
Tiny blood vessels in the retina can leak or rupture due to high blood sugar, resulting in:
- Blurred vision
- Retinal detachment
- Blindness, if untreated
5. Kidneys (Diabetic Nephropathy)
The kidneys’ filtering units (nephrons) are sensitive to high glucose levels:
- Leads to protein leakage into urine
- Can progress to chronic kidney disease or renal failure
6. Skin and Extremities
Poor circulation and nerve damage can cause:
- Slow-healing wounds
- Infections
- Foot ulcers (sometimes leading to amputation)
7. Brain and Mental Health
Diabetes is associated with:
- Increased risk of stroke
- Possible links to dementia and cognitive decline
- Emotional effects like depression and anxiety, partly due to chronic stress of managing the disease
8. Immune System
High blood sugar weakens white blood cells, making it harder for the body to:
- Fight infections
- Heal wounds quickly
9. Endocrine and Metabolic Effects
Insulin resistance disrupts the balance of other hormones, potentially affecting:
- Weight regulation
- Appetite
- Reproductive health (especially in women with PCOS or gestational diabetes)
Management Overview
Managing diabetes goes far beyond simply lowering blood sugar levels. It involves taking a comprehensive approach to maintain overall health, prevent complications, and improve quality of life. Successful management requires ongoing attention to diet, physical activity, medication, and regular monitoring all tailored to the individual’s needs and circumstances. For many people, building a plan for natural blood sugar control is an important starting point, alongside medical care.
Goals of Care
The primary goals of diabetes care are to maintain stable blood sugar levels, prevent complications, and support overall well-being. Effective management aims to balance medical treatment with lifestyle changes that promote long-term health and quality of life.
- Keep blood sugar within the target range: Maintaining blood glucose at safe levels helps prevent both short-term symptoms (such as fatigue and frequent urination) and long-term complications (such as kidney or nerve damage).
- Protect the heart, kidneys, eyes, and nerves: Since diabetes can damage blood vessels and organs, the goal is to control blood pressure, cholesterol, and blood sugar together. This reduces the risk of heart disease, stroke, kidney failure, vision problems, and nerve damage.
- Maintain a good quality of life: Diabetes care should enable individuals to live well, stay active, and manage their condition without it overwhelming daily life. Emotional well-being and stress management are important parts of this goal.
Shared Decision-Making and Team Approach
Effective diabetes management is best achieved through collaboration. Patients work closely with:
- Doctors oversee treatment and monitor complications.
- Diabetes educators to learn self-care skills and understand their condition.
- Dietitians to develop personalized meal plans that support balanced nutrition.
- Other healthcare providers as needed, such as pharmacists or mental health professionals.
This team approach ensures that care plans are realistic, individualized, and adjusted as the patient’s needs change. The patient plays an active role in decision-making, setting goals that are achievable and meaningful to their lifestyle.
Follow-Up and Review
Regular follow-ups typically every 3 to 6 months are essential. These visits help to:
- Review blood sugar levels, blood pressure, and cholesterol results.
- Adjust medications or insulin dosages if necessary.
- Detect and manage complications early.
- Reinforce lifestyle habits and provide ongoing education and support.
Healthy Living and Self-Management in Diabetes
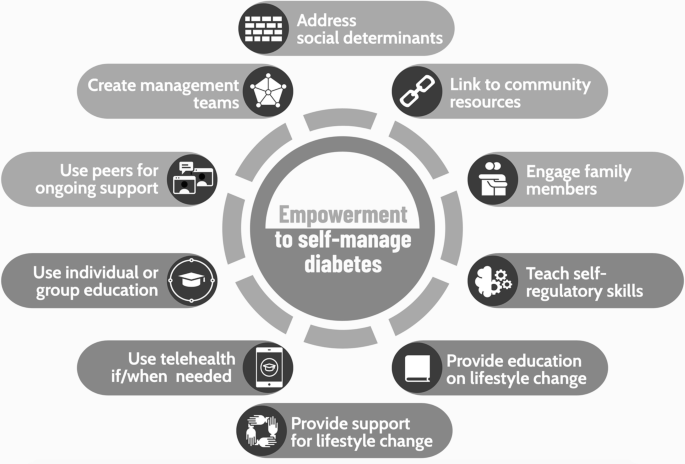
Lifestyle changes are the cornerstone of effective diabetes care. They not only help regulate blood sugar but also improve overall health, reduce the risk of complications, and enhance quality of life.
Healthy Eating
A balanced diet is essential in managing diabetes. Emphasis should be placed on vegetables, whole grains, lean proteins, and healthy fats. Dietary patterns such as the Mediterranean diet or plant-based diets have shown strong evidence for improving blood sugar levels and reducing cardiovascular risk. Portion control and mindful eating are also key strategies to prevent overeating and maintain stable glucose levels. Thoughtful meal planning and choosing the right foods for diabetes weight loss can help with both blood sugar and weight management.
Carbohydrate Quality
The type of carbohydrate consumed matters as much as the amount. It is important to choose high-fiber, low-glycaemic index foods such as legumes, whole grains, fruits, and non-starchy vegetables. Sugary beverages, refined grains, and processed snacks should be limited, as they can cause rapid spikes in blood sugar learning which foods to avoid with diabetes makes this much easier.
Physical Activity
Regular exercise improves insulin sensitivity and supports weight control. Individuals with diabetes should aim for at least 150 minutes of moderate-intensity physical activity per week (such as brisk walking, cycling, or swimming), combined with strength training at least twice a week. Even short, frequent bouts of movement throughout the day can be beneficial.
Weight Management
Achieving and maintaining a healthy weight significantly improves blood sugar regulation. Losing as little as 5–10 percent of body weight can enhance insulin sensitivity and reduce the need for medication. Structured lifestyle programs or, in some cases, bariatric surgery may be considered for individuals struggling with obesity or severe insulin resistance. Balanced nutrition paired with targeted recipes for diabetics with high cholesterol can support both weight and heart health.
Sleep, Stress, and Habits
Adequate sleep, stress reduction, and healthy daily habits all play a role in diabetes control. Poor sleep and chronic stress can raise blood sugar levels and disrupt hormone balance. Techniques such as relaxation exercises, mindfulness, and maintaining a consistent sleep schedule are helpful. Limiting alcohol intake and quitting smoking further decrease the risk of complications. For day-to-day stability, learning to manage blood sugar spikes after meals and during stress is especially important.
Oral Health
Oral hygiene is often overlooked but is crucial for people with diabetes. Gum disease (periodontitis) can worsen blood sugar control, and high glucose levels can increase susceptibility to infections. Regular dental check-ups, daily brushing, and flossing are important components of comprehensive diabetes care.
Medication Strategies in Diabetes Care
When lifestyle changes such as healthy eating and physical activity are not enough to maintain blood sugar within the target range, medications become a vital part of diabetes management. The type and combination of medicines depend on the kind of diabetes, individual health status, and treatment goals.
Type 1 Diabetes
People with Type 1 diabetes require daily insulin therapy because their bodies no longer produce insulin. Treatment typically involves a combination of:
- Long-acting insulin to maintain baseline (background) glucose control.
- Short-acting or rapid-acting insulin before meals to manage blood sugar spikes.
Insulin can be administered through multiple daily injections or via an insulin pump, which delivers continuous insulin throughout the day. Close monitoring of blood sugar levels and careful balancing of insulin doses with food intake and activity are essential to prevent both high and low blood sugar episodes.
Hypoglycemia Prevention
A major concern for individuals using insulin or certain oral medications is hypoglycemia (low blood sugar). It’s important to recognize early symptoms such as sweating, shakiness, confusion, or dizziness.
- Immediate treatment involves consuming glucose tablets, fruit juice, or sugary drinks.
- In severe cases, when the person cannot take oral sugar, glucagon (a hormone that raises blood sugar) can be administered by injection or nasal spray.
Education on prevention and emergency management is a critical part of diabetes care.
Type 2 Diabetes
For Type 2 diabetes, treatment often begins with metformin, the first-line medication that improves insulin sensitivity and reduces glucose production in the liver. When additional control or organ protection is needed, other classes of drugs may be added:
- GLP-1 receptor agonists (such as semaglutide or liraglutide) improve blood sugar control, promote weight loss, and protect the heart.
- SGLT2 inhibitors (such as empagliflozin or dapagliflozin) help the kidneys remove excess glucose and also offer heart and kidney protection.
- Additional options include DPP-4 inhibitors, thiazolidinediones (TZDs), and sulfonylureas, depending on the patient’s needs and tolerance.
If oral or injectable non-insulin medications are not sufficient, insulin therapy may be introduced.
Kidney Considerations
Since many diabetes medications are cleared through the kidneys, individuals with chronic kidney disease may require dose adjustments or alternative treatments to prevent toxicity and maintain safety. Regular monitoring of kidney function (eGFR and urine protein) helps guide medication choices.
Gestational Diabetes
For pregnant women with gestational diabetes, insulin is the preferred and safest treatment option, as it does not cross the placenta. However, in specific cases and under specialist supervision, certain oral medications such as metformin may be used. Strict blood sugar control during pregnancy helps protect both the mother and the baby from complications.
Preventing Complications and Staying Healthy
Preventing complications is just as important as managing blood sugar levels. Regular screening, vaccinations, and proactive care help protect long-term health and reduce the risk of serious diabetes-related problems.
Vaccinations
People with diabetes are more vulnerable to infections, making vaccination an essential part of preventive care. It is important to stay up to date with:
- Influenza (flu) vaccine : annually, to reduce seasonal infection risk.
- Pneumococcal vaccine : to prevent pneumonia and related complications.
- Hepatitis B vaccine : for protection against liver infection, especially in adults under 60 or with additional risk factors.
- COVID-19 vaccine and boosters : to lower the risk of severe illness.
Blood Pressure and Cholesterol
Managing blood pressure and cholesterol is key to protecting the heart and blood vessels.
- The goal is generally to keep blood pressure below 130/80 mmHg.
- Statins are often prescribed to lower cholesterol and reduce cardiovascular risk.
- ACE inhibitors or ARBs may be used to protect both the heart and kidneys.
Good control of these factors significantly decreases the chances of heart attack, stroke, and kidney disease.
Eye, Kidney, and Foot Checks
Routine screening detects complications early—before they cause lasting damage:
- Eye exams: Once a year to check for diabetic retinopathy or other eye changes.
- Kidney tests: Annual kidney function tests and urine checks for protein (microalbuminuria).
- Foot care: A foot check at every clinical visit and a comprehensive foot exam yearly to identify nerve damage, poor circulation, or ulcers early.
Sick-Day and Travel Tips
Special care is needed during illness or travel, as both can affect blood sugar control.
- Sick-day plan: Include instructions for checking glucose and ketones more frequently, adjusting medication, and staying hydrated.
- Travel preparation: Carry extra medication, insulin, testing supplies, and snacks. Keep a written list of prescriptions and emergency contacts.
- For long trips, adjust insulin timing if crossing time zones and store insulin properly.
Special Populations
Some groups need customized approaches to care.
- Older Adults: Simpler regimens, fewer side effects, and focus on maintaining independence.
- Adolescents: Early type 2 diabetes is rising in youth, so education and transition to adult care are critical.
- Pregnancy: Strict glucose control before and during pregnancy prevents complications.
- Resource-Limited Settings: Where access is limited, education, affordable drugs, and basic monitoring are priorities.
Emerging Trends & Research
The landscape of diabetes care is advancing rapidly.
- Diabetes Technology: Smart insulin pumps and continuous glucose monitoring systems make control easier and safer.
- New Therapies: Modern anti-obesity drugs and structured remission programs show promise in reversing early type 2 diabetes.
- Precision Medicine: Genetic and immune-based testing may allow earlier and more targeted prevention in the future.
Conclusion
Diabetes is a long-term metabolic disorder caused by insufficient insulin production or resistance, leading to high blood sugar. It can damage the heart, kidneys, eyes, nerves, and other organs if uncontrolled. The main types are Type 1, Type 2, and Gestational diabetes. Early detection through regular screening helps prevent complications. Effective management combines healthy eating, regular exercise, weight control, medications like insulin or GLP-1/SGLT2 drugs, and consistent monitoring. Preventive care, including vaccinations and routine eye, kidney, and foot checks, ensures long-term health and better quality of life for individuals with diabetes.
FAQs
What is the difference between type 1 and type 2 diabetes?
Type 1 is an autoimmune condition requiring lifelong insulin from diagnosis, while Type 2 is linked to insulin resistance and may start with lifestyle changes or oral medicines.
What A1C level defines diabetes and what is my goal?
An A1C level of 6.5 percent or higher defines diabetes. Most people aim for around 7 percent, personalized by age, health status, and risk of complications.
Can type 2 diabetes be reversed?
Yes, remission is possible through significant weight loss and lifestyle change, including improved diet and physical activity, but ongoing monitoring is always needed.
How often should I check my sugar if I’m on oral medicine?
It depends on your care plan and blood sugar stability. Some check daily, others weekly, and your doctor will advise based on your specific therapy.
What is the best diet for diabetes?
A balanced diet with whole foods, lean protein, vegetables, and limited added sugars works best to control blood sugar and support heart health.
Do GLP-1 or SGLT2 drugs protect my heart and kidneys?
Yes, these modern medications have been proven to lower risks of heart disease and kidney damage in people with Type 2 diabetes effectively.
What are the warning signs of DKA or HHS?
Very high sugar, excessive thirst, rapid breathing, fruity breath, confusion, or severe dehydration require immediate emergency care to prevent complications.
How often should I have eye, kidney, and foot exams?
Eye and kidney tests should be done yearly, and foot checks at every visit to detect early complications and prevent long-term damage.
What vaccines do I need?
Flu, pneumococcal, hepatitis B, and COVID-19 vaccines are recommended to reduce infection risks and maintain overall health in diabetes.
How should diabetes be managed in pregnancy?
With careful planning, regular monitoring, a healthy diet, and safe medication use under specialist supervision for both mother and baby’s safety.
Reference
- World Health Organization (WHO): Diabetes Overview
https://www.who.int/news-room/fact-sheets/detail/diabetes - Centers for Disease Control and Prevention (CDC): Diabetes Basics
https://www.cdc.gov/diabetes/basics/diabetes.html - American Diabetes Association (ADA): Standards of Care in Diabetes 2025
https://diabetesjournals.org/care - National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK): Diabetes Information
https://www.niddk.nih.gov/health-information/diabetes - Mayo Clinic: Diabetes Symptoms and Causes
https://www.mayoclinic.org/diseases-conditions/diabetes/symptoms-causes/syc-20371444 - National Health Service (NHS, UK): Diabetes Overview
https://www.nhs.uk/conditions/diabetes/
Dr. Aaron Liu, MD, FACE, is an endocrinologist with 14 years of experience managing diabetes, insulin resistance, and metabolic disorders. He completed his medical training at Columbia University Vagelos College of Physicians and Surgeons and fellowship in Endocrinology at Mount Sinai Hospital. Dr. Liu’s expertise lies in integrating precision nutrition and advanced glucose monitoring for improved glycemic control. He has authored continuing education modules for the American Diabetes Association on lifestyle-based diabetes reversal.

