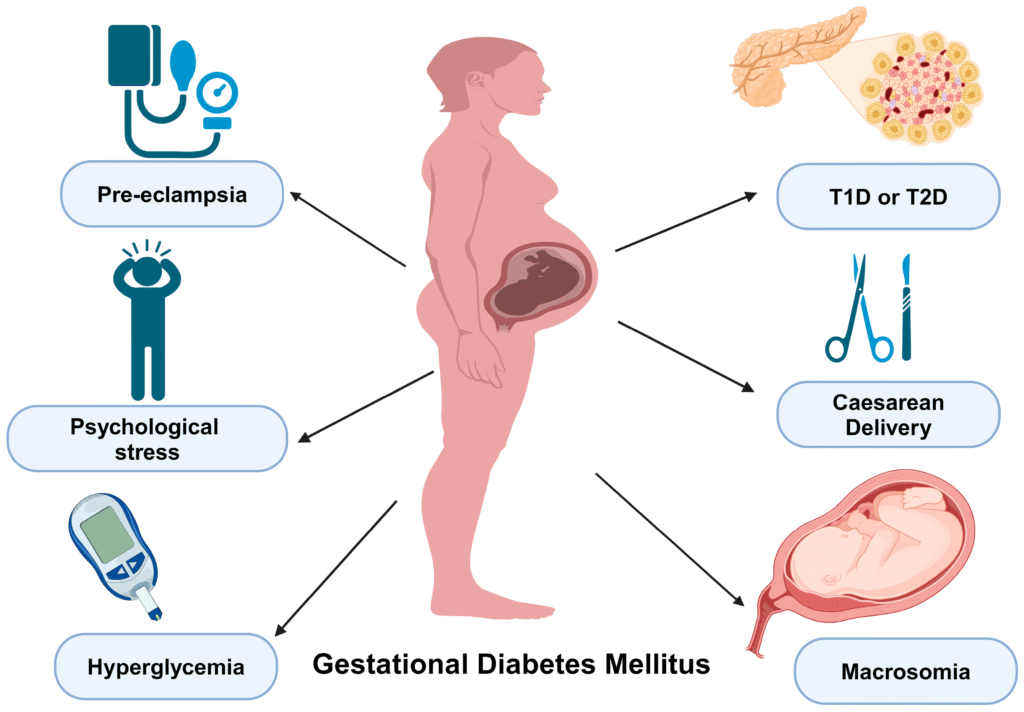
Gestational diabetes is a temporary but serious condition that develops during pregnancy when hormonal changes interfere with the body’s ability to regulate blood sugar effectively. This leads to elevated glucose levels that can impact both the mother and the growing baby. A balanced pregnancy diet is one of the most important tools in managing gestational diabetes, helping maintain stable blood sugar while supporting your baby’s healthy growth. With the right pregnancy diet, regular blood sugar monitoring, and healthy lifestyle habits, expectant mothers can manage gestational diabetes successfully and ensure a safe, healthy pregnancy for both themselves and their babies.
Key Takeaways
- A balanced, low glycemic pregnancy diet helps maintain stable blood sugar levels.
- Eating smaller, more frequent meals supports consistent energy and glucose control.
- Whole grains, lean proteins, fiber, and healthy fats are essential for both mother and baby.
- Staying active, hydrated, and mindful of portion sizes prevents glucose fluctuations.
- Regular prenatal checkups and blood sugar monitoring ensure safe pregnancy management.
What Is Gestational Diabetes During Pregnancy
Gestational diabetes (GDM) typically develops between the 24th and 28th weeks of pregnancy, when pregnancy hormones such as estrogen, progesterone, and cortisol reduce insulin sensitivity. This causes glucose to accumulate in the bloodstream instead of being used for energy.
While gestational diabetes often resolves after childbirth, it can increase the risk of complications such as:
- High birth weight (macrosomia)
- Preterm labor or cesarean delivery
- Preeclampsia (pregnancy related high blood pressure)
- A higher chance of developing type 2 diabetes later in life
Proper dietary management, exercise, and medical monitoring can keep blood sugar levels within a healthy range and reduce these risks.
Why Blood Sugar Control Matters During Pregnancy
Maintaining stable blood sugar levels is crucial for the health of both mother and baby. Uncontrolled gestational diabetes can lead to excessive growth of the baby, making delivery more difficult, and can cause low blood sugar in newborns after birth. High glucose levels also increase the risk of preterm labor, high blood pressure, and future metabolic issues for both mother and child.
Proper blood sugar management helps prevent complications such as preeclampsia, cesarean delivery, and postpartum recovery challenges. It also reduces the baby’s chances of developing obesity or Type 2 diabetes later in life. By following a balanced diet, staying active, and monitoring glucose levels regularly, expectant mothers can promote healthy fetal development and maintain their own well-being throughout pregnancy and beyond.
The Importance of a Healthy Pregnancy Diet

Nutrition plays a central role in managing gestational diabetes. A well balanced diet helps control blood sugar, supports the baby’s growth, and prevents excessive weight gain. The focus should be on consuming low glycemic, nutrient dense foods that digest slowly and provide steady energy throughout the day.
The goals of a healthy pregnancy diet are to:
- Maintain target blood glucose levels.
- Provide adequate nutrition for fetal growth and maternal health.
- Prevent blood sugar spikes and crashes.
- Support healthy weight gain during pregnancy.
Best Foods for Gestational Diabetes During Pregnancy
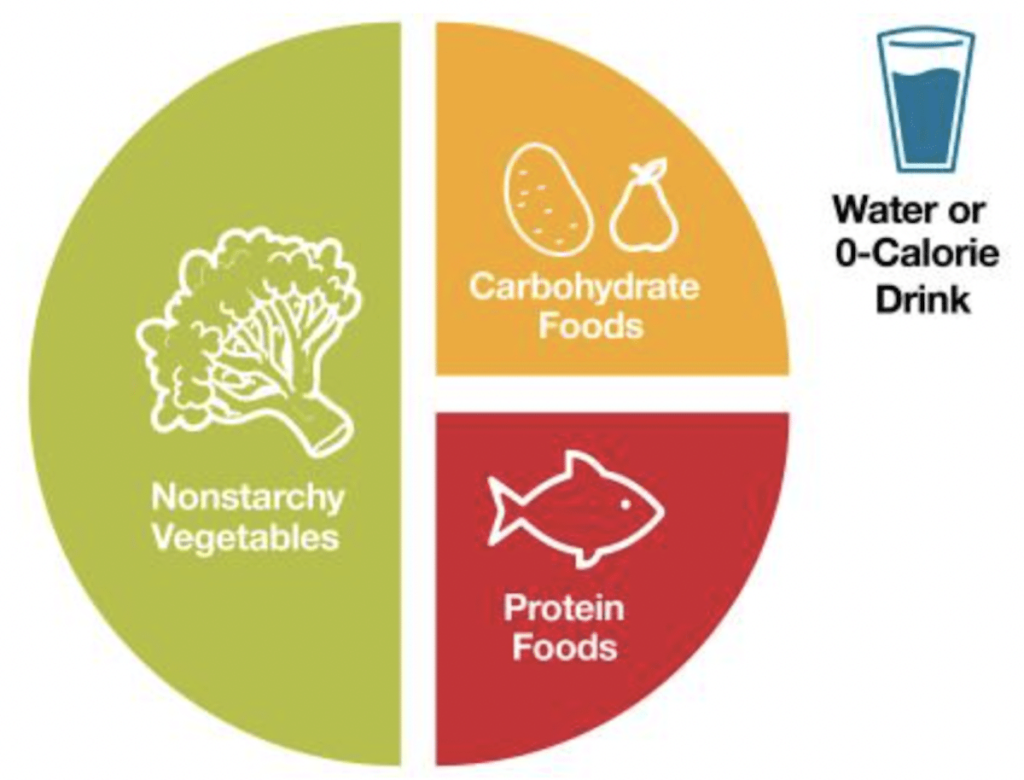
A well planned pregnancy diet should include foods that promote steady energy, optimal nutrition, and controlled blood sugar levels.
- Non Starchy Vegetables: Broccoli, spinach, kale, zucchini, cauliflower, and green beans are rich in fiber and vitamins while being low in carbohydrates.
- Lean Proteins: Choose skinless chicken, turkey, fish (like salmon), tofu, eggs, and lentils. These provide essential amino acids and help regulate blood sugar.
- Healthy Fats: Incorporate avocado, olive oil, chia seeds, flaxseeds, and nuts for heart healthy fats that also enhance satiety.
- Low Glycemic Fruits: Apples, berries, pears, and oranges can be enjoyed in moderation. Pair fruits with a protein source like nuts or Greek yogurt to reduce sugar spikes.
- Whole Grains and High Fiber Foods: Choose quinoa, barley, oats, or brown rice in small portions. These slow digesting carbohydrates help stabilize glucose levels.
- Low Fat Dairy or Alternatives: Greek yogurt, cottage cheese, and unsweetened almond milk offer calcium and protein without added sugars.
9 Key Nutrients for a Healthy Pregnancy with Gestational Diabetes
A balanced, nutrient-rich diet helps manage blood sugar levels, supports the baby’s growth, and promotes the mother’s health. Focusing on essential nutrients like fiber, protein, healthy fats, vitamins, and minerals ensures a healthy pregnancy and reduces complications.
1. Fiber
Fiber helps control blood sugar by slowing digestion and glucose absorption into the bloodstream. This prevents sudden spikes or drops in blood sugar after meals. It also promotes fullness, reducing overeating, and supports digestive health by preventing constipation. Fiber also nourishes healthy gut bacteria, which supports immune and metabolic balance.
Benefits for Gestational Diabetes:
- Improves insulin sensitivity so the body can use glucose effectively
- Reduces blood sugar spikes after meals
- Lowers LDL (“bad”) cholesterol and supports heart health
Rich Food Sources: Oats, lentils, apples, chia seeds, flaxseeds, beans, whole grains (brown rice, barley, quinoa), vegetables, and berries
Daily Target: 25–35 grams per day
Tip: Spread fiber intake across meals and drink plenty of water to prevent bloating.
2. Protein
Protein is the building block for the baby’s muscles, tissues, and organs. It also supports the mother’s metabolism, helps maintain lean muscle, and stabilizes blood sugar levels by slowing carbohydrate digestion.
Benefits for Gestational Diabetes:
- Keeps blood sugar steady between meals
- Reduces hunger and prevents overeating
- Supports fetal growth and maternal tissue repair
Rich Food Sources: Eggs, chicken, turkey, tofu, beans, lentils, fish (salmon, tilapia), lean meats, Greek yogurt, and cottage cheese
Daily Target: 70–100 grams per day, depending on body weight and doctor’s advice
Tip: Include a protein source with every meal or snack to maintain stable energy.
3. Calcium
Calcium is essential for the baby’s bone and tooth formation and supports the mother’s nerve, muscle, and cardiovascular functions. If the diet lacks calcium, the mother’s body draws it from her bones, leading to potential weakness later in life.
Benefits for Gestational Diabetes:
- Helps regulate insulin secretion
- Reduces risk of hypertension and preeclampsia
Rich Food Sources: Yogurt, milk, cheese, fortified plant-based milk (soy, almond, oat), broccoli, kale, and bok choy
Daily Target: 1,000–1,200 mg per day
Tip: Pair calcium-rich foods with vitamin D sources for better absorption.
4. Iron
Iron is needed to make hemoglobin, which carries oxygen through the blood to the mother and baby. During pregnancy, blood volume increases, heightening iron needs. Iron deficiency can cause anemia, fatigue, and developmental risks for the baby.
Benefits for Gestational Diabetes:
- Prevents anemia and supports oxygen transport
- Supports fetal and placental growth
Rich Food Sources: Lean meats (beef, turkey, chicken), spinach, kale, lentils, beans, and fortified cereals
Tip: Pair iron-rich foods with vitamin C sources (like oranges or bell peppers) to enhance absorption. Avoid tea or coffee around meals.
Daily Target: 27 mg per day
5. Omega-3 Fatty Acids
Omega-3s, especially DHA and EPA, are essential for the baby’s brain, eye, and nervous system development. They also reduce inflammation and support heart health in the mother.
Benefits for Gestational Diabetes:
- Improves insulin resistance
- Reduces inflammation and supports cardiovascular health
- May lower the risk of preterm birth and postpartum depression
Rich Food Sources: Salmon, sardines, mackerel, chia seeds, flaxseeds, walnuts, and omega-3 fortified eggs
Daily Target: 200–300 mg DHA per day, as advised by healthcare providers
Tip: Non-fish eaters can take algae-based omega-3 supplements under medical guidance.
6. Folate (Vitamin B9)
Folate supports DNA synthesis, cell division, and red blood cell production. It is crucial in early pregnancy to prevent neural tube defects (brain and spinal cord issues) in the baby.
Benefits for Gestational Diabetes:
- Supports placental growth and function
- Aids red blood cell production
- Promotes healthy tissue repair and fetal development
Rich Food Sources: Leafy greens (spinach, kale, collard greens), citrus fruits, avocados, lentils, beans, asparagus, and fortified cereals
Daily Target: 600 micrograms per day
Tip: Continue prenatal vitamins with folic acid as prescribed by your doctor.
7. Magnesium
Magnesium is involved in more than 300 biochemical processes, including blood sugar control, nerve signaling, and muscle relaxation. It also helps prevent leg cramps and supports better sleep and calmness.
Benefits for Gestational Diabetes:
- Improves insulin function and glucose control
- Reduces risk of high blood pressure and preeclampsia
- Promotes relaxation and healthy sleep
Rich Food Sources: Nuts (almonds, cashews), seeds (pumpkin, sunflower, chia), avocados, leafy greens, whole grains, and dark chocolate
Daily Target: 350–400 mg per day
Tip: Get magnesium mainly from food; supplements should be used only under medical supervision.
8. Vitamin D
Vitamin D supports calcium absorption and bone strength for both mother and baby. It also plays a role in immune health, hormone balance, and mood regulation. Many pregnant women are deficient, especially those with limited sunlight exposure.
Benefits for Gestational Diabetes:
- Improves insulin sensitivity and glucose balance
- Strengthens fetal bones and immune system
- May lower the risk of preeclampsia and mood disorders
Rich Food Sources: Fortified milk, eggs, salmon, tuna, mushrooms, and safe sunlight exposure (10–15 minutes daily)
Daily Target: 600–800 IU per day or more, as advised by a doctor
9. Zinc
Zinc is vital for DNA synthesis, immune function, and tissue growth. It supports the baby’s organ development and helps repair tissues in the mother. Zinc also contributes to insulin production and healthy metabolism.
Benefits for Gestational Diabetes:
- Aids insulin synthesis and blood sugar regulation
- Strengthens immunity
- Promotes fetal growth and tissue repair
Rich Food Sources: Pumpkin seeds, chickpeas, lentils, cashews, beef, eggs, and whole grains
Daily Target: 11–12 mg per day
Tip: Soak or sprout beans, grains, and seeds before cooking to enhance zinc absorption.
Foods to Avoid for Managing Gestational Diabetes in Pregnancy
Maintaining balanced blood sugar during pregnancy starts with mindful eating. Certain foods can raise glucose levels quickly, increase insulin resistance, or contribute to excess weight gain all of which heighten the risk of developing gestational diabetes. Limiting or avoiding these foods supports a healthier pregnancy for both mother and baby.
- Refined carbohydrates: White bread, white rice, pastries, and sugary cereals can cause sharp spikes in blood sugar. Choose whole grains like oats, quinoa, or brown rice instead.
- Sugary drinks and fruit juices: Beverages like soda, sweetened tea, and packaged fruit juices contain large amounts of sugar with no fiber. Stick to water, infused water, or unsweetened herbal tea.
- Processed and fried foods: Chips, fries, and fast food meals are high in unhealthy fats and refined carbs that can worsen insulin resistance.
- Desserts and sweets: Cakes, cookies, candy, and sweetened snacks quickly elevate glucose levels and provide little nutrition.
- High fat dairy and processed meats: Full fat cheese, sausages, bacon, and deli meats can raise cholesterol and inflammation, increasing metabolic strain.
- Sweetened yogurts and flavored milk: These often contain hidden sugars, choose plain, unsweetened Greek yogurt or milk alternatives.
- Caffeinated and energy drinks: Excess caffeine can interfere with glucose control and affect the baby’s development, keep intake minimal.
- Packaged snacks high in sodium: High salt intake can elevate blood pressure and contribute to fluid retention during pregnancy.
- Unpasteurized dairy and soft cheeses: Avoid infections that can complicate pregnancy and affect overall maternal health.
Healthy Lifestyle Tips for Managing Gestational Diabetes
In addition to following a balanced pregnancy diet, adopting healthy lifestyle habits plays a crucial role in maintaining stable blood sugar levels, supporting your baby’s growth, and ensuring a smooth pregnancy journey. These small, consistent changes can make a big difference:
- Eat smaller, frequent meals: Divide your meals into 5-6 smaller portions throughout the day to keep glucose levels steady and prevent sudden spikes or drops.
- Balance every meal: Combine complex carbohydrates with lean proteins and healthy fats to slow glucose absorption and sustain energy levels.
- Incorporate regular physical activity: Engage in light to moderate exercises such as brisk walking, prenatal yoga, or swimming (with doctor’s approval). These activities enhance insulin sensitivity and reduce stress.
- Stay well hydrated: Drink 6-8 glasses of water daily to support kidney function and help flush out excess glucose.
- Prioritize good sleep: Aim for 7-9 hours of quality rest each night. Poor sleep can disrupt hormonal balance, increase stress hormones, and raise blood sugar levels.
- Manage stress effectively: Stress hormones like cortisol can raise blood sugar, so practice relaxation techniques such as deep breathing, meditation, or gentle stretching.
- Avoid skipping meals: Skipping meals can cause blood sugar fluctuations and increase hunger cravings later.
- Monitor blood sugar regularly: Follow your doctor’s advice for checking glucose levels at home. Tracking readings helps you understand how your diet and activity affect your blood sugar.
- Plan ahead for snacks: Keep healthy options like nuts, fruit with nut butter, or whole grain crackers handy to prevent hunger between meals.
When to Consult Your Doctor
Regular prenatal checkups are essential for tracking both your health and your baby’s development. However, if you notice unusual symptoms or changes, it’s important to contact your healthcare provider promptly.
Seek medical advice if you experience:
- Consistently high or low blood sugar readings despite following your diet plan.
- Excessive fatigue, dizziness, or weakness that doesn’t improve with rest.
- Frequent thirst or urination, especially if it disrupts your sleep.
- Sudden weight gain, swelling, or shortness of breath.
- Blurred vision or severe headaches.
- Reduced baby movement or unusual fetal activity.
- Nausea or vomiting that affects your ability to eat or stay hydrated.
Conclusion
Gestational diabetes occurs when pregnancy hormones affect insulin function, raising blood sugar levels. A balanced, nutrient rich diet is key to managing this condition and supporting a healthy pregnancy. Focusing on low glycemic foods, lean proteins, whole grains, and healthy fats helps maintain stable glucose and promote fetal growth. Eating smaller, frequent meals, staying active, hydrated, and managing stress all contribute to healthy blood sugar control. Regular prenatal checkups and glucose monitoring ensure both mother and baby remain safe. With mindful eating and consistent habits, expectant mothers can effectively manage gestational diabetes and enjoy a smooth, healthy pregnancy journey.
FAQs
What is gestational diabetes?
Gestational diabetes is a temporary condition that develops during pregnancy when hormones affect how your body uses insulin, leading to high blood sugar levels.
Can gestational diabetes harm my baby?
If left unmanaged, it can increase the risk of a larger than average baby, premature birth, or low blood sugar after delivery but with proper diet and monitoring, most pregnancies remain healthy.
What foods should I focus on during pregnancy with gestational diabetes?
Include lean proteins, high fiber vegetables, whole grains, healthy fats, and low glycemic fruits in moderate portions to maintain steady blood sugar.
Are fruits safe to eat with gestational diabetes?
Yes, choose low glycemic fruits such as apples, pears, and berries, and pair them with a protein source like yogurt or nuts to avoid sugar spikes.
How often should I eat during the day?
Eat smaller, balanced meals every 3-4 hours. This helps maintain stable glucose levels and prevents energy crashes.
Can I exercise with gestational diabetes?
Absolutely. Light to moderate activities like walking or prenatal yoga (with your doctor’s approval) help improve insulin sensitivity and overall health.
Is insulin always required for gestational diabetes?
Not necessarily. Many women manage it through diet and exercise alone. However, if blood sugar remains high, your doctor may recommend insulin therapy.
Can gestational diabetes go away after childbirth?
In most cases, blood sugar returns to normal after delivery, but you’ll need follow up testing as it may increase your future risk of type 2 diabetes.
How much water should I drink daily?
Aim for 6-8 glasses of water each day to stay hydrated, support digestion, and help regulate blood sugar naturally.
Can gestational diabetes be prevented?
While not always preventable, maintaining a healthy weight, staying active, managing stress, and following a balanced pregnancy diet before and during pregnancy can lower your risk.
References
Bevan, Catherine. “How to Prevent Gestational Diabetes: 4 Tips for a Healthy Pregnancy.” Baylor Scott & White Health, https://www.bswhealth.com/blog/4-ways-to-help-prevent-gestational-diabetes., Accessed 10 Nov. 2025.
Shah, Dr. Ami. “Diet for Gestational Diabetes: What to Eat & What to Avoid.” PharmEasy, 1 Jul. 2025,
https://pharmeasy.in/conditions/diet-for-gestational-diabetes-indian-what-to-eat-what-to-avoid/, Accessed 10 Nov. 2025.
Warwick, Kathy W. “Gestational Diabetes Diet: Foods to Eat and Avoid.” Medical News Today, https://www.medicalnewstoday.com/articles/319716#foods-to-eat., Accessed 10 Nov. 2025.
Dr. Aaron Liu, MD, FACE, is an endocrinologist with 14 years of experience managing diabetes, insulin resistance, and metabolic disorders. He completed his medical training at Columbia University Vagelos College of Physicians and Surgeons and fellowship in Endocrinology at Mount Sinai Hospital. Dr. Liu’s expertise lies in integrating precision nutrition and advanced glucose monitoring for improved glycemic control. He has authored continuing education modules for the American Diabetes Association on lifestyle-based diabetes reversal.

