Checking blood sugar helps people with diabetes manage their condition, avoid complications, and adjust treatment effectively. The testing frequency depends on the type of diabetes, treatment plan, and how stable the blood sugar levels are.
Key Takeaways
- Type 1 diabetics usually test 4–10 times daily or use a Continuous Glucose Monitor (CGM).
- Type 2 diabetics on insulin test multiple times daily, while others test a few times weekly.
- Gestational diabetes requires around four tests a day, typically fasting and after meals.
- Factors like illness, stress, and medication changes may need extra testing.
- Tracking results regularly helps identify patterns and supports better glucose control.
Why Blood Sugar Monitoring Is Important

Monitoring blood sugar is one of the most important daily habits for anyone living with diabetes. It gives a clear picture of How Often to Check for Diabetes and how different choices or situations affect blood sugar levels. Without regular checks, it becomes difficult to notice sudden changes that could lead to health problems.
Key Benefits of Regular Monitoring
When you test your blood sugar, you’re gathering information that helps both you and your healthcare team make smarter decisions. Each reading tells you how your body reacts to food, medicine, stress, and physical activity. Over time, these readings show patterns that can guide better treatment and lifestyle choices.
- Prevents low or high blood sugar episodes: Frequent testing helps you catch unusual spikes or drops early, allowing you to take quick action before they become dangerous.
- Tracks how medications are working: Blood sugar readings show if your current insulin dose or diabetes medicine is effective or needs adjustment.
- Supports smart food and activity choices: By comparing readings before and after meals or exercise, you can see what foods or activities help maintain balance.
- Lowers the risk of long-term complications: Consistent monitoring helps you keep glucose within a healthy range, reducing the risk of nerve damage, kidney disease, and vision problems in the future
How Often to Check for Diabetes : Type 1
People with Type 1 diabetes need to check blood sugar often because their body doesn’t make insulin, and levels can change quickly with food, exercise, or stress. Regular testing helps keep glucose within a safe range and guides insulin use.
Most people use a glucometer or a continuous glucose monitor (CGM) to track levels accurately.
Recommended Testing Times
- Before meals and snacks to guide insulin doses
- Before and after exercise to prevent low blood sugar
- Before bedtime to ensure safe nighttime levels
- Occasionally during the night if levels tend to drop
- When feeling sick or stressed since both can raise glucose
This usually adds up to 4 to 10 checks per day. A CGM makes it easier by giving real-time readings and alerts for sudden changes.
How Often to Check for Diabetes : Type 2
People with Type 2 diabetes do not all need to check their blood sugar at the same frequency. The right schedule depends on the type of treatment, how stable the readings are, and what the doctor recommends. Regular testing helps you understand how meals, medicine, and activity affect your blood sugar and gives you control over your daily decisions.
Testing also helps detect changes early, so you can prevent complications and adjust your care plan when needed. The main goal is to keep your blood sugar within a healthy range throughout the day.
If on Insulin
When insulin is part of the treatment, blood sugar levels can rise or fall quickly, so frequent checks are necessary to stay safe and avoid hypoglycemia.
- Check before meals and at bedtime, usually three to four times a day
- Test more often when changing insulin doses or if blood sugar levels fluctuate
- Include occasional post-meal checks to see how food affects glucose control
If on Oral Medication
People taking tablets such as metformin or sulfonylureas may not need to test as often as those on insulin, but regular monitoring still provides valuable feedback.
- Test once or twice a day, or a few times per week as your doctor advises
- Try testing at different times, such as before breakfast one day and after dinner another, to identify patterns
- Use results to understand how different meals or activities change your readings
If Managing Through Diet and Exercise
Those who manage Type 2 diabetes through lifestyle changes alone can usually test less often, but it’s still helpful to see how choices affect glucose levels.
- Check a few times per week, especially before and after main meals
- Test after new foods or workouts to learn how they influence your readings
- Keep a simple log to track changes over time and share with your healthcare provider
Even with good control, periodic testing helps ensure that blood sugar remains steady and that your plan continues to work well.
How Often to Check for Gestational Diabetes
Gestational diabetes occurs during pregnancy and requires close monitoring to protect both the mother and baby. Regular testing helps doctors ensure that blood sugar stays within the target range and that any changes in diet or insulin are effective.
Since pregnancy can make blood sugar fluctuate quickly, frequent checks provide the information needed to adjust meal plans and keep energy levels stable.
Typical schedule for gestational diabetes:
- Take a fasting test each morning before breakfast
- Check one or two hours after each meal to see how food affects glucose
This usually equals four checks per day. More frequent testing may be necessary if your readings are not within target or if insulin treatment begins. Regular monitoring supports a healthy pregnancy and reduces the risk of complications during birth.
How to Perform a Blood Sugar Test Correctly
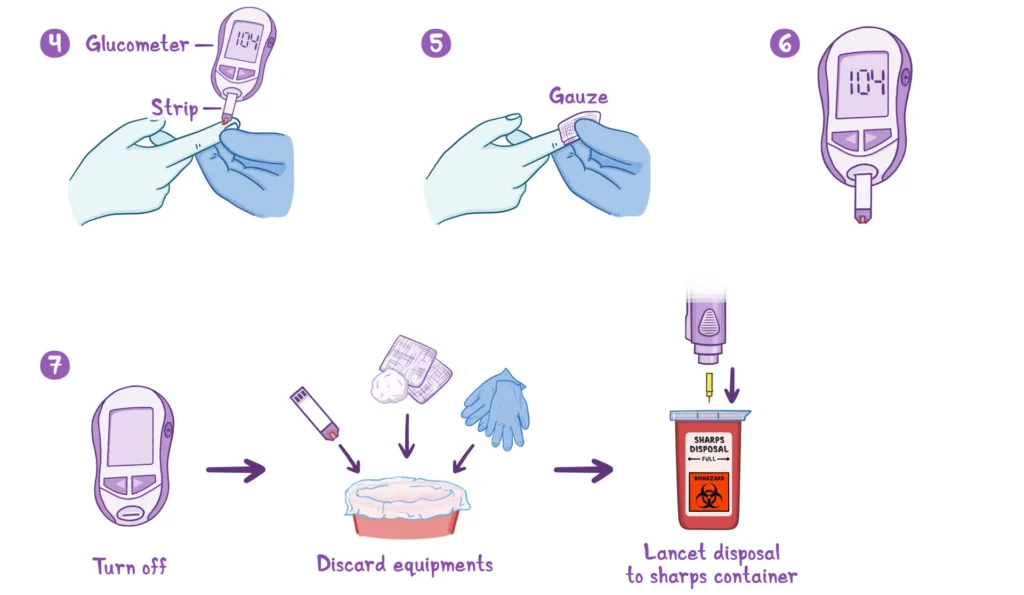
Accurate testing is essential for managing diabetes effectively. A few careful steps can make sure every reading reflects your true blood sugar level and not simple errors during the process.
- Wash and dry your hands completely: Warm water helps improve blood flow, and clean hands prevent contamination that can alter results.
- Use a new lancet each time: Reusing lancets can make pricks more painful and increase the risk of infection.
- Prick the side of the fingertip: It’s less sensitive than the center and provides enough blood for testing.
- Place the blood drop correctly on the test strip: Avoid pressing or squeezing too hard, which can affect accuracy.
- Record the reading immediately: Note the time, value, and any factors like meals, medication, or activity.
- Dispose of strips and lancets safely: Use a sharps container or other secure disposal method.
Factors That Affect Testing Frequency
How often you check blood sugar depends on your health, lifestyle, and treatment plan: Some people need frequent testing, while others can test less often. These key factors help decide the right schedule.
- Type of diabetes and treatment method: People using insulin need more frequent checks than those managing with tablets or diet.
- Stability of glucose control: Unstable readings require more frequent monitoring.
- Age and overall health : Older adults or those with other health conditions may need closer checks.
- Physical activity level : Exercise can lower blood sugar, so testing before and after activity is useful.
- Stress or illness : Both can raise blood sugar, making extra testing important.
- Changes in medication or routine : New treatments or daily schedule changes can affect glucose levels.
Using Continuous Glucose Monitors (CGMs)
A Continuous Glucose Monitor (CGM) is a small wearable device that tracks blood sugar levels automatically throughout the day and night. It measures glucose from the fluid under the skin and sends data to a phone or reader, showing patterns and trends without frequent finger pricks.
- Real-time updates every few minutes to show changing glucose levels
- Alerts for high or low readings so action can be taken quickly
- Better tracking of food and activity effects to guide daily decisions
Even with a CGM, occasional finger-stick tests are still needed to confirm accuracy or recalibrate the device.
When to Test More Frequently
At certain times, it’s important to check blood sugar more often than usual. Extra testing helps catch sudden changes early and prevents both high and low glucose levels from becoming serious. These checks are temporary but essential for staying safe and maintaining good control.
- Starting or changing diabetes medication to see how the body responds
- Feeling dizzy, shaky, or unusually tired which may signal low or high blood sugar
- Being sick, injured, or under stress since these can raise glucose unexpectedly
- Traveling, especially across time zones when meal and medication schedules change
- During pregnancy or when planning pregnancy to keep blood sugar within the safest range
Understanding and Recording Your Results
Tracking blood sugar readings helps identify patterns and gives doctors accurate data to adjust treatment. It shows how meals, exercise, and medication affect glucose control.
Useful tracking tips
- Record the date, time, and glucose reading for each test
- Note meals, exercise, stress, or symptoms that may affect results
- Use a digital meter or mobile app for automatic logging
Typical target ranges for most adults (ADA guidelines)
- Before meals: 80–130 mg/dL
- 1–2 hours after meals: Below 180 mg/dL
These targets may vary depending on age, health, and treatment plan, so confirm your personal range with your doctor.
When to Contact Your Doctor
Even with regular blood sugar monitoring, there are times when professional help is needed. Some changes in your readings or symptoms may signal that your diabetes plan requires adjustment. Knowing when to call your doctor helps prevent complications and keeps your blood sugar under safe control.
- Repeated readings above 250 mg/dL or below 70 mg/dL despite following your usual routine. These levels can be dangerous if not corrected.
- Symptoms of very high or low blood sugar, such as confusion, dizziness, blurred vision, or excessive thirst.
- Persistent morning highs even when you’re eating well and taking medication as prescribed. This may indicate the need for a change in dosage or timing.
- Difficulty understanding or interpreting your results, especially if readings seem inconsistent or unpredictable.
Conclusion
Regular blood sugar testing is essential for effective diabetes management. The right frequency depends on the type of diabetes, medication, and how stable glucose levels are. Type 1 diabetics usually test 4–10 times daily or use a CGM, while Type 2 may test from several times a day to a few times weekly depending on treatment. Gestational diabetes often requires four daily checks. Testing more often is needed during illness, stress, or medication changes. Tracking results helps identify patterns, guide adjustments, and maintain healthy, stable blood sugar control.
FAQs
How often should I check my blood sugar if I have Type 1 diabetes?
People with Type 1 diabetes usually need to check their blood sugar 4 to 10 times a day. Testing before meals, snacks, exercise, bedtime, and sometimes overnight helps keep levels within a safe range. A Continuous Glucose Monitor (CGM) can make this easier by tracking readings automatically.
How often should I check if I have Type 2 diabetes?
The frequency depends on your treatment:
- On insulin: 3–4 times a day (before meals and at bedtime)
- On oral medication: once or twice daily or a few times per week
- Diet and exercise only: a few times per week, mainly before and after meals
How often should I check blood sugar during pregnancy with gestational diabetes?
Most women with gestational diabetes test four times daily once before breakfast (fasting) and after each main meal. Your doctor may recommend more frequent checks if insulin is required or readings are unstable.
What is the best time of day to test blood sugar?
Common testing times include:
- Before meals to guide medication or insulin doses
- 1–2 hours after meals to check how food affects glucose
- Before bedtime to ensure safe overnight levels
- Before and after exercise or when feeling unwell
Do I still need to test if I feel fine and my readings are usually normal?
Yes. Even if you feel well, regular testing helps detect changes early and keeps track of long-term control. Some blood sugar changes happen without obvious symptoms.
Can I rely only on a Continuous Glucose Monitor (CGM)?
A CGM gives real-time glucose data and alerts for highs and lows, but you should occasionally confirm readings with a finger-stick test to ensure accuracy and recalibrate the device when needed.
How can I make blood sugar testing less painful?
- Use a new lancet each time
- Prick the side of your fingertip, not the center
- Rotate fingers to avoid soreness
- Consider lancing devices with adjustable depth settings
What should I do if my readings are very high or very low?
If your blood sugar is above 250 mg/dL or below 70 mg/dL, recheck to confirm and take corrective action as directed by your doctor. If it doesn’t improve or you feel unwell, contact your healthcare provider immediately.
How can I track my blood sugar results effectively?
Keep a logbook or use a mobile app that records readings automatically. Include date, time, meals, exercise, and any symptoms. Reviewing these logs with your doctor helps fine-tune your treatment.
What long-term tests show how well my blood sugar is controlled?
The A1C test measures your average blood sugar over the past 2–3 months. Most adults should aim for below 7%, but your target may vary. Daily monitoring supports this goal by keeping day-to-day levels steady.
Reference
- Centers for Disease Control and Prevention (CDC). Manage Blood Sugar. https://www.cdc.gov/diabetes/managing/manage-blood-sugar.html
- Mayo Clinic. Blood Glucose Monitors: What Factors Affect Accuracy? https://www.mayoclinic.org/diseases-conditions/diabetes/in-depth/blood-glucose-monitors/art-20050988
- Diabetes UK. Checking Your Blood Sugar Levels. https://www.diabetes.org.uk/guide-to-diabetes/managing-your-diabetes/testing
- MedlinePlus. Blood Glucose Test. https://medlineplus.gov/lab-tests/blood-glucose-test/
- Medscape. Self-Monitoring of Blood Glucose in Diabetes Management. https://www.medscape.com/viewarticle/915514
- World Health Organization (WHO). Diabetes Management and Care Guidelines. https://www.who.int/news-room/fact-sheets/detail/diabetes
Dr. Aaron Liu, MD, FACE, is an endocrinologist with 14 years of experience managing diabetes, insulin resistance, and metabolic disorders. He completed his medical training at Columbia University Vagelos College of Physicians and Surgeons and fellowship in Endocrinology at Mount Sinai Hospital. Dr. Liu’s expertise lies in integrating precision nutrition and advanced glucose monitoring for improved glycemic control. He has authored continuing education modules for the American Diabetes Association on lifestyle-based diabetes reversal.

