Type 2 diabetes is a chronic condition that affects how the body processes blood sugar (glucose). It develops gradually, often going unnoticed for years until symptoms become more severe. Recognizing the Symptoms of Type 2 Diabetes is crucial for timely diagnosis, effective management, and preventing long-term complications.
Key Takeaways
- Type 2 diabetes often develops slowly and may not cause obvious symptoms at first.
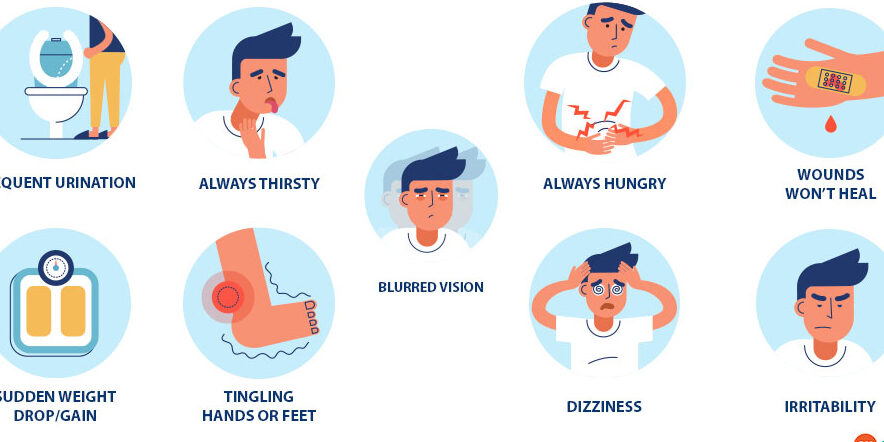
- Common early warning signs include excessive thirst, frequent urination, fatigue, and slow wound healing.
- Unexplained weight changes, blurred vision, and frequent infections may also indicate rising blood sugar levels.
- Early diagnosis and lifestyle management can help control blood sugar and prevent serious complications.
What Is Type 2 Diabetes?
Type 2 diabetes happens when the body becomes resistant to insulin, the hormone that helps move sugar from the bloodstream into cells or when the pancreas doesn’t make enough insulin. As a result, glucose builds up in the blood instead of being used for energy.
This form of diabetes is largely linked to genetics, age, obesity, and lifestyle factors such as poor diet and physical inactivity. Over time, high blood sugar can damage major organs including the heart, kidneys, nerves, and eyes, making early detection and control essential.
Why Early Detection Matters
Type 2 diabetes develops gradually, and early symptoms can be easy to miss. Feeling unusually tired or thirsty might seem minor, but they can signal rising blood sugar. Detecting it early helps prevent complications like nerve damage, vision problems, and heart disease. Simple lifestyle changes, diet, exercise, and medication can make a big difference.
Early Warning Signs and Symptoms of Type 2 Diabetes

Type 2 diabetes often develops slowly, and early signs can be subtle. Paying attention to changes in your body can help detect the condition before complications arise.
Excessive Thirst and Frequent Urination (Polydipsia and Polyuria)
High blood sugar forces the kidneys to work overtime to filter and excrete excess glucose. When glucose levels exceed the kidney’s threshold, sugar spills into the urine, drawing water along with it through a process called osmotic diuresis. This leads to frequent urination (polyuria) and dehydration, which in turn causes excessive thirst (polydipsia). This symptom cycle urinate more, drink more is a classic early warning sign of diabetes.
Increased Hunger (Polyphagia)
Despite high glucose in the bloodstream, cells are unable to absorb it efficiently due to insulin deficiency or resistance. Because the cells are starved for energy, the body sends hunger signals to the brain to encourage eating. As a result, you may feel hungry soon after meals or experience persistent cravings, even though the body already has excess glucose it can’t use properly.
Fatigue and Weakness
Glucose is the body’s main energy source, but when insulin isn’t functioning effectively, glucose remains in the blood instead of entering the cells. The body then turns to fat and muscle stores for fuel, leading to energy depletion and metabolic inefficiency. This causes persistent fatigue, weakness, and a lack of stamina even after adequate sleep or food intake.
Blurred Vision
Elevated blood sugar levels can cause the lens of the eye to swell as fluid moves in and out of it, temporarily changing its shape and flexibility. This results in blurred or fluctuating vision. Over time, prolonged high glucose can damage retinal blood vessels, leading to diabetic retinopathy, a serious complication that threatens long-term vision.
Slow-Healing Wounds and Frequent Infections
Chronic high blood sugar impairs circulation and weakens immune cell function, reducing the body’s ability to fight infections and repair tissues. Cuts, bruises, and wounds heal slowly, and infections particularly skin, urinary tract, and gum infections become more common. Poor blood flow also means less oxygen reaches tissues, further delaying recovery and increasing the risk of ulcers.
Unexplained Weight Loss or Gain
When the body can’t utilize glucose for energy, it begins to break down fat and muscle to fuel itself, causing unintended weight loss despite normal or increased appetite. Conversely, some individuals experience weight gain as the body produces more insulin in response to resistance, leading to fat storage, especially around the abdomen.
Tingling or Numbness in Hands and Feet (Peripheral Neuropathy)
Prolonged exposure to high blood sugar damages the nerves and blood vessels that supply them. This leads to peripheral neuropathy, characterized by tingling, burning sensations, numbness, or pain especially in the hands and feet. Over time, this can affect coordination, reflexes, and even lead to injuries going unnoticed.
Darkened Skin Patches (Acanthosis Nigricans)
Excess insulin in the bloodstream stimulates the overgrowth of skin cells and increases pigment production. This results in thickened, velvety, darkened patches commonly found on the neck, armpits, groin, or elbows. Though not harmful, acanthosis nigricans is a visible marker of insulin resistance and an early sign of metabolic imbalance.
Frequent Yeast or Fungal Infections
Excess sugar in tissues creates an ideal environment for yeast (Candida) and other fungi to thrive. These infections often occur in warm, moist areas like the mouth, genitals, under skin folds, or between fingers. They may recur frequently unless blood sugar levels are properly controlled.
Mood Changes and Irritability
Fluctuating glucose levels can affect the brain’s energy supply and neurotransmitter balance, leading to mood swings, irritability, anxiety, and difficulty concentrating. Chronic hyperglycemia can also contribute to long-term changes in brain chemistry, increasing the risk of depression and cognitive decline if not managed effectively.
Others Symptoms in Different Age Groups
Type 2 diabetes can affect people of all ages, but symptoms may appear differently depending on your stage of life. Understanding these variations helps in spotting the condition early and taking timely action.
Children and Teenagers:
Children and teens may not always clearly express how they feel, making it important for parents and caregivers to watch for changes in behavior or health.
- Increased Thirst and Frequent Bathroom Trips: High blood sugar causes the kidneys to work harder, leading to constant urination and persistent thirst.
- Unusual Fatigue or Irritability: Energy levels drop as the body struggles to use glucose, often making children appear unusually tired or cranky.
- Weight Gain or Dark Skin Patches: Insulin resistance can cause rapid weight gain or velvety, darkened skin, especially around the neck or armpits.
- Slow-Healing Cuts or Frequent Infections: Elevated blood sugar weakens the immune system, leading to longer recovery from minor injuries or recurrent infections.
Adults (20–60 Years):
Adults may overlook subtle symptoms for months or even years, so paying attention to small changes in energy, vision, or sensation is crucial.
- Constant Tiredness: Persistent fatigue occurs because glucose isn’t being used efficiently for energy.
- Blurred Vision: High blood sugar can temporarily distort vision, making it difficult to focus clearly.
- Tingling or Numbness: Nerve damage from prolonged elevated sugar levels may cause tingling, burning, or numbness in the hands and feet.
- Slow Wound Healing: Cuts or sores may take longer to heal due to impaired circulation and immune response.
Older Adults (60+ Years):
Symptoms in seniors may be mistaken for normal aging, which can delay diagnosis and treatment.
- Fatigue or Confusion: Low energy and occasional confusion may signal high blood sugar affecting overall brain function.
- Unexplained Weight Loss: Weight loss without changes in diet or activity can occur as the body starts using fat and muscle for energy.
- Frequent Infections: Recurring urinary tract, skin, or gum infections are common due to weakened immunity.
- Vision Problems or Dizziness: Fluctuating glucose levels can affect eyesight and balance, increasing the risk of falls.
When to Seek Medical Attention

It’s important to consult a doctor if you notice any of the following signs, as they may indicate rising blood sugar or early diabetes:
- Persistent thirst or frequent urination: High blood sugar makes the kidneys work harder, leading to dehydration and constant need to drink or urinate.
- Sudden vision changes: Blurred or fluctuating vision can occur when glucose levels affect the lens of the eye.
- Numbness or tingling in hands or feet: Tingling, burning, or numbness may be an early sign of nerve damage caused by prolonged high blood sugar.
- Unexplained fatigue or weight changes: Feeling unusually tired or noticing sudden weight loss or gain can signal that the body isn’t using glucose properly.
- Slow-healing wounds or frequent infections: Cuts, bruises, or infections that take longer to heal can indicate impaired immunity due to high blood sugar.
- Recurrent yeast or urinary infections: Excess sugar creates an environment for yeast and bacteria to grow, leading to repeated infections.
Early screening through simple blood glucose tests can confirm diabetes or prediabetes, allowing timely lifestyle changes and treatment to prevent complications.
Risk Factors That Increase Chances of Type 2 Diabetes
Certain factors make developing type 2 diabetes more likely:
- Family History of Diabetes: Having a parent or sibling with diabetes increases your risk.
- Being Overweight or Obese: Excess body fat, especially around the abdomen, can cause insulin resistance.
- Sedentary Lifestyle: Lack of regular physical activity reduces the body’s ability to use insulin effectively.
- High Blood Pressure or Cholesterol: Cardiovascular risk factors often accompany insulin resistance.
- Polycystic Ovary Syndrome (PCOS): Women with PCOS are at higher risk due to hormonal imbalances affecting insulin.
- Poor Diet High in Refined Sugars and Fats: Frequent consumption of sugary drinks, processed foods, and fried items increases risk.
- History of Gestational Diabetes: Women who had diabetes during pregnancy are more likely to develop type 2 diabetes later in life.
Prevention and Early Management
Adopting healthy habits can significantly lower your risk or help manage early diabetes:
- Stay Active: Aim for at least 30 minutes of moderate exercise most days, including walking, cycling, or strength training.
- Eat Smart: Focus on nutrient-rich foods like whole grains, vegetables, fruits, lean proteins, and healthy fats, while limiting sugary snacks and processed foods.
- Maintain a Healthy Weight: Even losing 5–7% of your body weight can improve insulin sensitivity and lower your risk.
- Get Regular Screenings: Blood glucose and HbA1c tests help detect diabetes early, especially if you have risk factors or a family history.
- Manage Stress: Chronic stress can raise blood sugar levels; practices like yoga, meditation, or mindful breathing help maintain balance.
- Prioritize Sleep: Poor sleep patterns can affect insulin sensitivity, so aim for 7–9 hours per night.
- Limit Alcohol and Quit Smoking: Both can increase the risk of diabetes and related complications.
Conclusion
Type 2 diabetes often develops quietly, with early symptoms that can easily be overlooked. Signs like fatigue, frequent thirst, blurred vision, or slow-healing wounds should never be ignored, as early recognition allows for timely intervention. Understanding your personal risk factors and adopting healthy habits such as regular exercise, a balanced diet, maintaining a healthy weight, managing stress, and getting adequate sleep can prevent or delay the onset of diabetes. Regular screenings and prompt medical attention for unusual symptoms are essential to protect your heart, kidneys, nerves, and eyes from long-term complications. Awareness, early detection, and proactive lifestyle choices remain the most effective tools in managing and preventing type 2 diabetes.
FAQs
What is type 2 diabetes?
Type 2 diabetes is a condition where the body becomes resistant to insulin or doesn’t produce enough insulin, leading to high blood sugar levels.
What are the early signs of type 2 diabetes?
Early signs include frequent urination, excessive thirst, unusual fatigue, blurred vision, slow-healing wounds, and unexplained weight changes.
Can type 2 diabetes be prevented?
Yes, maintaining a healthy weight, staying active, eating a balanced diet, managing stress, avoiding smoking, and regular screenings can significantly reduce risk.
Is type 2 diabetes reversible?
In some cases, with early diagnosis, lifestyle changes, and weight management, blood sugar levels can return to normal, a state called remission.
Who is at higher risk for type 2 diabetes?
People with a family history of diabetes, overweight or obese individuals, those with a sedentary lifestyle, or women with a history of gestational diabetes or PCOS are at higher risk.
How often should I get tested for diabetes?
Adults over 35 or those with risk factors should get tested every 1–3 years. If you have symptoms, consult a doctor immediately.
Can stress cause type 2 diabetes?
Chronic stress increases hormones like cortisol, which can raise blood sugar and contribute to insulin resistance.
Is blurred vision caused by diabetes permanent?
Not usually. Controlling blood sugar often improves vision, but prolonged high sugar levels can cause permanent eye damage if untreated.
What complications can arise from untreated type 2 diabetes?
Untreated diabetes can lead to heart disease, kidney damage, nerve damage (neuropathy), vision loss, and increased risk of infections.
What lifestyle changes help manage type 2 diabetes?
Regular exercise, a healthy diet, maintaining a healthy weight, managing stress, adequate sleep, limiting alcohol, and avoiding smoking are key steps in managing blood sugar effectively.
References
NHS (National Health Service). Symptoms of type 2 diabetes and how it’s diagnosed. Available at:https://www.nhs.uk/conditions/type-2-diabetes/symptoms/ Accessed: 6 November 2025.
Healthdirect. Type 2 diabetes – symptoms, causes and treatment. Available at: https://www.healthdirect.gov.au/type-2-diabetes? Accessed: 6 November 2025.
Cleveland Clinic. Type 2 Diabetes: What It Is, Causes, Symptoms & Treatment. Available at: https://my.clevelandclinic.org/health/diseases/21501-type-2-diabetes Accessed: 6 November 2025.
Medical News Today. 9 early warning signs and symptoms of type 2 diabetes. Available at: https://www.medicalnewstoday.com/articles/323185 Accessed: 6 November 2025.
Dr. Aaron Liu, MD, FACE, is an endocrinologist with 14 years of experience managing diabetes, insulin resistance, and metabolic disorders. He completed his medical training at Columbia University Vagelos College of Physicians and Surgeons and fellowship in Endocrinology at Mount Sinai Hospital. Dr. Liu’s expertise lies in integrating precision nutrition and advanced glucose monitoring for improved glycemic control. He has authored continuing education modules for the American Diabetes Association on lifestyle-based diabetes reversal.

