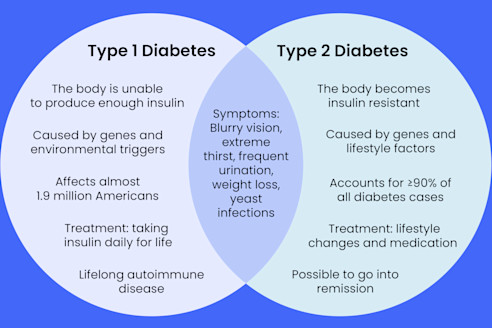
Diabetes affects millions of people worldwide, but not all types are the same. Type 1 and Type 2 diabetes are two forms of a chronic condition that affect how the body regulates blood sugar (glucose), its main energy source. Although both lead to high blood sugar levels, their causes, onset, and treatment differ significantly. Understanding these differences helps in early detection, effective management, and prevention of serious health complications.
Key Takeaways
- Type 1 diabetes results from an autoimmune reaction where the body stops producing insulin.
- Type 2 diabetes develops when the body becomes insulin resistant or doesn’t produce enough insulin.
- Type 1 usually develops early in life, while Type 2 appears gradually, often after age 40.
- Type 1 requires lifelong insulin therapy, while Type 2 can often be managed through diet, exercise, and medication.
- Early diagnosis and lifestyle changes can help control blood sugar and prevent complications.
What Are Type 1 and Type 2 Diabetes?
Type 1 diabetes is an autoimmune condition where the body’s immune system attacks and destroys the insulin producing beta cells in the pancreas. Without insulin, glucose cannot enter the cells for energy, leading to dangerously high blood sugar. This type develops suddenly, often in children, teens, or young adults, and requires lifelong insulin therapy through injections or an insulin pump.
Type 2 diabetes, on the other hand, develops when the body becomes resistant to insulin or the pancreas cannot produce enough of it. It progresses gradually and is strongly linked to obesity, poor diet, inactivity, and genetics. Type 2 is the most common form, accounting for about 90-95% of all diabetes cases, and can often be prevented or reversed with early intervention and lifestyle changes.
How Insulin Works in the Body
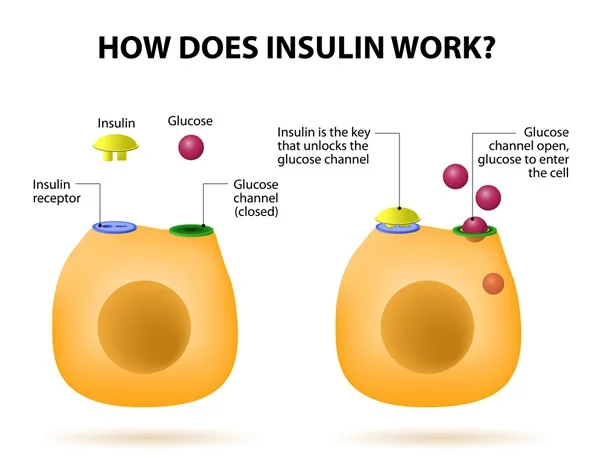
Insulin is a vital hormone produced by the beta cells in the pancreas, specifically in an area called the Islets of Langerhans. Its main job is to help the body use or store glucose, the sugar derived from the food we eat. After eating, carbohydrates are broken down into glucose, which enters the bloodstream and causes blood sugar levels to rise. In response, the pancreas releases insulin, which acts like a key that unlocks the body’s cells (especially in muscles, fat, and the liver) so that glucose can enter and be used for energy. Any excess glucose that isn’t immediately needed is stored in the liver and muscles as glycogen or converted into fat for later use. When blood sugar levels drop for example, between meals or during physical activity insulin levels decrease, allowing the body to release stored glucose to maintain balance.
Insulin in Type 1 Diabetes
In people with Type 1 diabetes, the immune system mistakenly attacks and destroys these insulin producing beta cells. Without insulin, glucose cannot enter the cells and instead builds up in the bloodstream. This leads to dangerously high blood sugar levels and forces the body to rely on fat as an alternative energy source, which produces ketones acids that can lead to a life threatening condition known as diabetic ketoacidosis (DKA). Because the pancreas no longer produces insulin, people with Type 1 diabetes need daily insulin injections or an insulin pump to survive and maintain stable glucose levels.
Insulin in Type 2 Diabetes
In Type 2 diabetes, the body still makes insulin, but the cells stop responding to it properly, a problem called insulin resistance. This means glucose can’t enter the cells easily and builds up in the blood. To make up for this, the pancreas works harder and produces more insulin. Over time, this extra effort tires out the insulin producing cells, causing insulin levels to drop and blood sugar to rise. This process usually happens slowly, often over many years, and may not cause symptoms at first. Factors like unhealthy eating habits, lack of exercise, being overweight, and stress play a big role in developing insulin resistance.
Main Differences Between Type 1 and Type 2 Diabetes

While both type 1 and type 2 diabetes cause high blood sugar, they differ in how they develop, who they affect, and how they’re treated. Type 1 results from the immune system attacking insulin producing cells, while type 2 develops gradually due to insulin resistance. Knowing these differences helps with early detection and effective management.
| Feature | Type 1 Diabetes | Type 2 Diabetes |
| Cause | Autoimmune destruction of insulin producing cells | Insulin resistance and reduced insulin production |
| Age of Onset | Sudden, usually in children or young adults | Gradual, often after age 40 |
| Insulin Production | Little or none | Reduced or ineffective |
| Treatment | Insulin injections or pump | Diet, exercise, oral meds, or insulin |
| Body Weight | Often normal or underweight | Often overweight or obese |
| Prevention | Not preventable | Can often be prevented or delayed |
| Family History | Less common | More common |
| Frequency | About 5-10% of all diabetes cases | About 90-95% of all diabetes cases |
Common Symptoms of Type 1 and Type 2 Diabetes
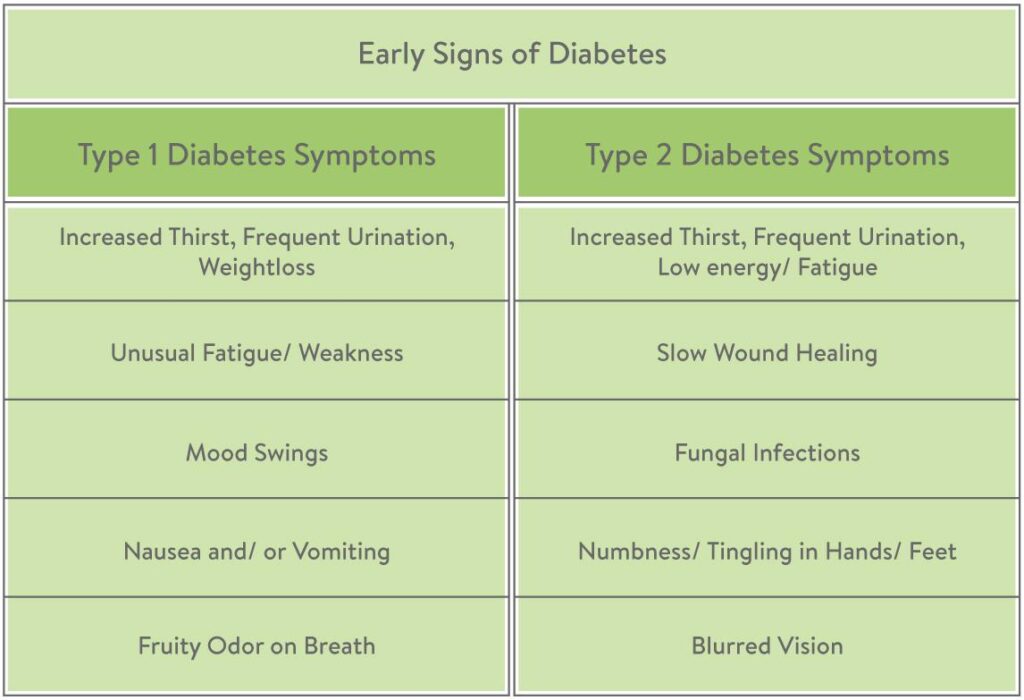
Both type 1 and type 2 diabetes share similar warning signs caused by elevated blood sugar levels. Recognizing these symptoms early is essential for timely diagnosis and treatment. High glucose levels affect how the body uses energy and can impact multiple organs, leading to noticeable physical changes and discomfort. Common symptoms include:
- Frequent urination and excessive thirst
- Extreme hunger or fatigue
- Unexplained weight changes
- Blurred vision
- Slow healing wounds or frequent infections
- Numbness or tingling in hands and feet
Causes and Risk Factors
The causes and risk factors for diabetes vary depending on the type. Type 1 diabetes is primarily linked to autoimmune reactions and genetic factors, while Type 2 diabetes is strongly influenced by lifestyle, diet, and body weight.
For Type 1 Diabetes
Type 1 diabetes often develops when the immune system mistakenly attacks insulin producing cells in the pancreas. While the exact cause isn’t fully understood, certain factors can increase the risk:
- Family history of autoimmune diseases
- Genetic predisposition
- Autoimmune conditions like thyroid or celiac disease
- Viral infections triggering immune reactions
- Low vitamin D levels or limited sunlight exposure
- Geographic factors more common in colder regions
For Type 2 Diabetes
Type 2 diabetes is largely preventable and develops over time due to insulin resistance and poor lifestyle habits. Several factors raise the risk of developing it:
- Being overweight or obese
- Sedentary lifestyle with little physical activity
- Poor diet high in sugar and refined carbohydrates
- Family history of diabetes
- High blood pressure or cholesterol
- Polycystic Ovary Syndrome (PCOS) or gestational diabetes
- Chronic stress or inadequate sleep
- Age over 40 (though increasingly seen in younger adults)
How Type 1 and Type 2 Diabetes Are Identified
Diabetes is diagnosed through specific blood tests that measure glucose levels and assess how the body produces or uses insulin. While both types involve high blood sugar, the methods used to confirm each condition differ slightly.
Type 1 Diabetes
Because Type 1 diabetes develops suddenly and involves the immune system destroying insulin producing cells, diagnosis focuses on identifying both high blood sugar and autoimmune activity in the body.
- Fasting blood glucose or HbA1c test shows very high sugar levels.
- Autoantibody tests confirm that the immune system is attacking insulin producing cells.
- C peptide test checks how much insulin the pancreas is still producing (usually very low).
- Ketone tests may detect ketones in the urine or blood, common in Type 1 diabetes.
- Symptoms such as sudden weight loss, fatigue, excessive thirst, and frequent urination appear quickly, often within weeks.
Type 2 Diabetes
Type 2 diabetes develops more gradually, so diagnosis aims to detect persistently elevated blood sugar and signs of insulin resistance before complications arise.
- Fasting blood glucose, HbA1c, or oral glucose tolerance test shows consistently elevated sugar levels over time.
- Doctors assess insulin resistance, cholesterol, and blood pressure to understand metabolic health.
- Gradual symptom onset such as tiredness, blurred vision, or slow healing wounds often leads to testing.
- Type 2 diabetes is sometimes discovered during routine checkups since early signs can be mild or unnoticed.
Long Term Complications of Diabetes
If either Type 1 or Type 2 diabetes is not well controlled, it can lead to serious long term complications that affect many parts of the body. Over time, high blood sugar can damage blood vessels and nerves, increasing the risk of several health problems:
- Heart and blood vessel disease: People with diabetes have a higher risk of heart attack, stroke, and high blood pressure due to damage to the arteries.
- Kidney damage (nephropathy): High glucose levels can harm the kidneys filtering system, which may eventually lead to kidney failure or the need for dialysis.
- Nerve damage (neuropathy): Excess sugar can injure nerves throughout the body, causing tingling, numbness, burning, or pain especially in the hands and feet.
- Eye problems (retinopathy): Damage to the blood vessels in the eyes can lead to blurred vision, vision loss, or even blindness if left untreated.
- Foot complications: Poor blood flow and nerve damage can cause ulcers and infections that may take longer to heal.
- Skin and oral issues: People with diabetes are more prone to skin infections, gum disease, and dry or itchy skin.
How to Manage Type 1 and Prevent Type 2 Diabetes

Managing and preventing diabetes involves maintaining stable blood sugar levels, adopting healthy habits, and following a consistent medical plan. While Type 1 diabetes cannot be prevented, it can be well managed with proper care. Type 2 diabetes, however, is largely preventable through lifestyle changes and early intervention.
Type 1 Diabetes
Since Type 1 diabetes is an autoimmune condition, management focuses on replacing insulin and maintaining a healthy lifestyle to balance blood sugar.
- Take insulin regularly through injections or an insulin pump as prescribed.
- Monitor blood glucose several times a day using a glucometer or continuous glucose monitor (CGM).
- Follow a balanced diet that includes complex carbs, lean proteins, and healthy fats.
- Exercise regularly to improve energy levels and insulin sensitivity, with doctor guidance.
- Manage stress through mindfulness, yoga, or breathing exercises to reduce glucose fluctuations.
- Stay consistent with medical checkups to monitor for complications and adjust insulin doses.
Type 2 Diabetes
Type 2 diabetes can often be prevented or even reversed in its early stages by maintaining a healthy lifestyle and addressing risk factors early.
- Maintain a healthy weight through regular exercise and portion controlled meals.
- Eat nutrient dense foods, such as vegetables, whole grains, fruits, and lean proteins.
- Limit sugar and refined carbs that cause blood sugar spikes.
- Exercising at least 150 minutes per week, brisk walking, swimming, or cycling are excellent choices.
- Monitor blood sugar levels regularly, especially if you have risk factors.
- Avoid smoking and limit alcohol, which can worsen insulin resistance.
- Manage blood pressure, cholesterol, and stress for better metabolic health.
- Get regular screenings to detect early changes in blood sugar or insulin resistance.
Conclusion
Diabetes affects millions worldwide, but Type 1 and Type 2 differ greatly in cause and management. Type 1 is an autoimmune disease in which the body stops producing insulin, requiring lifelong insulin therapy. Type 2 develops when the body becomes resistant to insulin or produces too little, often linked to lifestyle factors like obesity, diet, and inactivity. While Type 1 cannot be prevented, Type 2 can often be delayed or reversed through healthy habits, exercise, and weight control. Recognizing early symptoms and maintaining balanced blood sugar are vital for preventing complications and living a healthy, active life.
FAQs
What is the main difference between Type 1 and Type 2 diabetes?
Type 1 diabetes is an autoimmune disease where the body stops producing insulin, while Type 2 diabetes occurs when the body becomes resistant to insulin or doesn’t produce enough of it.
Who is more likely to develop Type 1 diabetes?
Type 1 diabetes typically develops in children, teens, or young adults and is not caused by lifestyle factors but by genetic and autoimmune triggers.
Can Type 2 diabetes be reversed?
Yes, in many cases, early stage Type 2 diabetes can be reversed through weight loss, healthy eating, and regular exercise that improve insulin sensitivity.
What are early signs of diabetes?
Common symptoms include frequent urination, excessive thirst, fatigue, blurred vision, slow healing wounds, and unexplained weight changes.
Is Type 1 diabetes preventable?
No, Type 1 diabetes cannot be prevented because it results from an autoimmune reaction, but it can be effectively managed with insulin and a healthy lifestyle.
How is diabetes diagnosed?
Doctors use blood tests such as fasting glucose, HbA1c, and glucose tolerance tests to measure blood sugar levels and identify the type of diabetes.
What foods should people with diabetes avoid?
It’s best to limit sugary drinks, refined carbs, processed snacks, and fried foods that can cause blood sugar spikes and increase insulin resistance.
How often should blood sugar be checked?
People with Type 1 diabetes should monitor it multiple times a day, while those with Type 2 should follow their doctor’s recommendations usually a few times per week or daily if on medication.
What happens if diabetes is left untreated?
Uncontrolled diabetes can lead to heart disease, kidney failure, nerve damage, vision loss, and an increased risk of infections.
Can exercise help control diabetes?
Absolutely. Regular physical activity improves insulin sensitivity, lowers blood sugar levels, and supports healthy weight management for both Type 1 and Type 2 diabetes.
References
“Differences between type 1 and type 2 diabetes.” Diabetes UK, https://www.diabetes.org.uk/diabetes-the-basics/differences-between-type-1-and-type-2-diabetes,
Accessed 9 Nov. 2025.
Huston, Kim. “Type 1 vs Type 2 diabetes differences.” Norton Children’s, 13 Nov. 2019, https://nortonchildrens.com/news/type-1-vs-type-2-diabetes/,
Accessed 9 Nov. 2025.
Wood, Kelly. “Type 1 vs. Type 2 Diabetes: Difference, Symptoms, and More.” Healthline, 27 Mar. 2025, https://www.healthline.com/health/difference-between-type-1-and-type-2-diabetes#prevention,
Accessed 9 Nov. 2025.
Wood, Kelly. “Type 1 vs. Type 2 diabetes: What are the differences?” MedicalNewsToday, 26 Feb. 2025, https://www.medicalnewstoday.com/articles/7504,
Accessed 9 Nov. 2025.
Dr. Aaron Liu, MD, FACE, is an endocrinologist with 14 years of experience managing diabetes, insulin resistance, and metabolic disorders. He completed his medical training at Columbia University Vagelos College of Physicians and Surgeons and fellowship in Endocrinology at Mount Sinai Hospital. Dr. Liu’s expertise lies in integrating precision nutrition and advanced glucose monitoring for improved glycemic control. He has authored continuing education modules for the American Diabetes Association on lifestyle-based diabetes reversal.

