
Postmenopausal women’s bone health declines quickly after menopause as estrogen falls, accelerating bone breakdown and raising osteoporosis and fracture risk. Early screening, strength-building exercise, adequate calcium and vitamin D, and targeted treatment preserve mobility for years.
Key takeaways
- Estrogen decline after menopause is the main trigger for accelerated bone loss and higher osteoporosis risk in women.
- Many women have no symptoms until a fracture occurs, making bone density testing (DEXA scan) essential.
- Core prevention pillars: adequate calcium, vitamin D, and protein plus regular weight-bearing and resistance exercise.
- Major risk factors: age over 50, early or surgical menopause, family history, low BMI, smoking, alcohol, inactivity, and long-term steroid use.
- Treatment options include hormone replacement therapy and non-hormonal osteoporosis medications to reduce fracture risk.
- Fall prevention, home safety, and routine bone health checkups are critical to protect independence in older women.
Why Bone Health Changes After Menopause
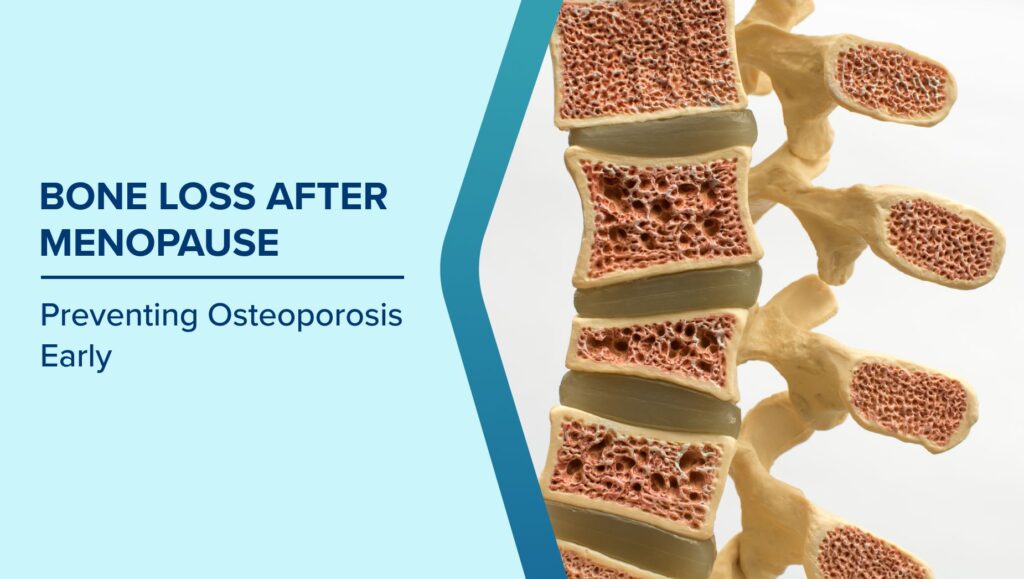
Bones are living tissue that renews itself throughout life. Specialized cells called osteoclasts break down old bone, while osteoblasts build new bone to replace it. In younger women, this remodeling cycle stays balanced, so bone density remains steady and the skeleton keeps its strength and resilience.
After menopause, Postmenopausal Bone Health shifts because estrogen levels drop sharply. Estrogen normally slows bone resorption and supports bone formation, but once it declines, osteoclast activity speeds up while rebuilding lags behind. This causes faster bone loss in women and a measurable fall in menopause and bone density, especially in the hips, spine, and wrists areas most vulnerable to osteoporosis-related fractures.
Estrogen’s Role in Women’s Bone Health

Estrogen is a key regulator of bone turnover, acting like a control switch that keeps breakdown and rebuilding in balance. In healthy women’s skeletal health, estrogen supports osteoblasts (bone-building cells), restrains osteoclasts (bone-breaking cells), and helps preserve bone structure. After menopause, estrogen levels fall sharply, and the bone-remodeling system tips toward faster loss. This accelerates bone loss in women and lowers menopause and bone density, especially in the spine and hips, making postmenopausal bone health a critical focus.
Estrogen helps regulate bone remodeling by:
- Maintaining bone-building cell activity
- Slowing the breakdown of bone tissue
- Supporting calcium absorption
- Protecting the structural integrity of bones
When estrogen levels fall, the entire bone-building system becomes imbalanced, causing rapid declines in bone density, skeletal strength, and bone integrity.
Without intervention, this leads to:
- Loss of bone mass
- Increased fracture risk
- Structural weakening of the spine
- Height loss and spinal curvature
Osteoporosis in Women
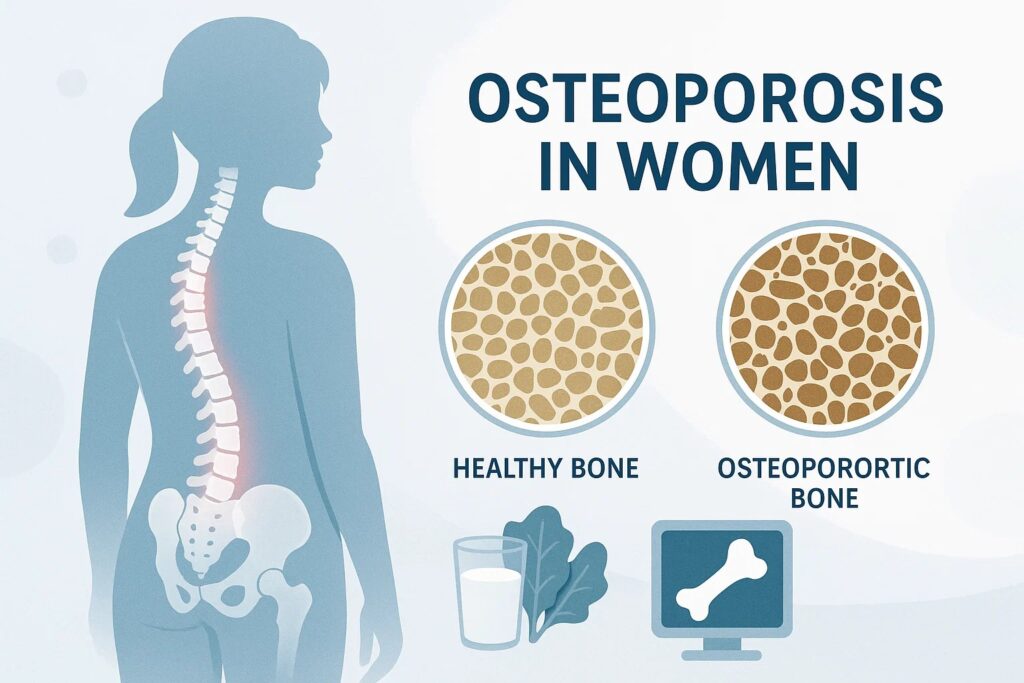
Osteoporosis in women is a condition where bones become porous and fragile, increasing fracture risk. Because it develops silently, many women don’t notice any warning signs until a minor fall causes a wrist, spine, or hip fracture. This makes early attention to postmenopausal bone health essential.
Common osteoporosis risk factors include:
- Early menopause (before 45) or surgical removal of ovaries
- Family history of osteoporosis or hip fractures
- Low body weight/BMI
- Smoking and frequent alcohol use
- Long-term steroid use (e.g., prednisone)
- Thyroid disorders, diabetes, rheumatoid arthritis, malabsorption issues
Common Symptoms of Bone Loss in Postmenopausal Women
Bone loss after menopause is often called a “silent” problem because it can progress for years without obvious pain. Still, subtle physical changes may show up as bones thin and spinal support weakens. Noticing these early signs can help women seek testing and care before a major fracture occurs.
- Loss of height
- Stooped posture
- Back pain or spinal tenderness
- Weak or brittle nails
- Frequent fractures or breakage from minor impact
- Reduced grip strength
Causes and Risk Factors for Bone Loss in Women
Bone loss after menopause comes from a mix of hormonal shifts, health conditions, and lifestyle habits. If you have one or more risk factors, your chances of postmenopausal bone loss are higher
Hormonal & medical factors
Hormones and certain health conditions strongly influence how fast bones break down. After menopause, lower estrogen removes a key layer of protection, and some illnesses or medicines can speed up bone thinning even more.
- Early menopause (before 45) or surgical removal of ovaries
- Family history of osteoporosis or hip fracture
- Long-term steroid use (e.g., prednisone)
- Thyroid or parathyroid disorders
- Conditions such as rheumatoid arthritis, celiac disease, or chronic kidney disease
Lifestyle factors
Daily habits play a huge role in how well your bones stay strong. Poor nutrition, low activity, and harmful substances can quietly weaken bones over years, especially after menopause when bone loss is already faster.
- Low calcium or vitamin D intake
- Physical inactivity
- Smoking
- Heavy alcohol use
- Low body weight or rapid weight loss
- Poor sleep and chronic stress (linked to higher inflammation and hormonal disruption)
Age-related factors
Aging naturally changes bone and muscle metabolism. Over time, the body builds less new bone, muscles weaken, and balance declines making both bone loss and fall risk higher.
- Aging reduces bone formation and muscle mass, increasing fall risk and accelerating bone mineral density (BMD) decline
How to Improve Bone Density After Menopause

You can’t change your age or menopause status, but you can change the direction your bones take from here. The most effective approach is a combo of nutrition, targeted exercise, and lifestyle support, sometimes with medication if fracture risk is high.
1. Calcium and Vitamin D for Women
Calcium is the main mineral that builds bone, and vitamin D helps your body absorb and use it properly. Most guidelines recommend meeting your needs through food first, and using supplements only when diet or sunlight isn’t enough.
- Milk, yogurt, cheese
- Fortified soy/almond/oat milk
- Tofu made with calcium salts
- Sardines and salmon with bones
- Kale, bok choy, broccoli
- Almonds, sesame, chickpeas
Recommended intake
- Calcium: 1,200 mg/day for women over 50.
- Vitamin D: 800-1,000 IU/day if sun exposure or diet is low.
2. Weight-Bearing Exercise for Bones
Weight-bearing activities make your skeleton carry your body weight against gravity, which signals bones to stay dense. Doing these most days of the week helps slow bone loss and supports balance and muscle strength.
- Brisk walking or hiking
- Stair climbing
- Dancing
- Jogging or jump training if joints allow
3. Resistance Training to Improve BMD(Bone Mineral Density)
Strength training applies direct load to bone through muscles, making it one of the most reliable ways to improve or preserve BMD after menopause. Programs 2-3 days a week at moderate-to-high intensity are especially effective for spine and hip density.
- Squats, lunges, step-ups
- Deadlifts / hip hinges
- Rows, push-ups, overhead presses
4. Balance and Fall Prevention
Strong bones help, but preventing falls is just as important because most fractures happen after slipping or tripping. Balance training improves coordination and reaction time, lowering fracture risk.
- Tai chi or yoga
- Single-leg stands
- Core and hip stability work
5. Lifestyle Habits for Strong Bones
Daily habits can either protect or quietly weaken your skeleton. Supporting muscle, sleep, and metabolism helps keep bone remodeling healthier and reduces long-term loss.
- Stop smoking (weakens bone and estrogen pathways)
- Limit alcohol (heavy intake reduces bone formation)
- Sleep 7-9 hours consistently
- Keep a stable, healthy body weight
- Eat adequate protein for muscle support
Hormone Replacement Therapy (HRT)
Hormone Replacement Therapy (HRT), also called menopausal hormone therapy, replaces estrogen (and progesterone if you still have a uterus). By restoring estrogen after menopause, it slows bone resorption, helps preserve bone mineral density (BMD), and reduces osteoporosis related fracture risk, especially at the spine and hip when started soon after menopause.
HRT is mainly recommended for women in early postmenopause who also need relief from symptoms like hot flashes, since bone protection is a major added benefit. It is not suitable for everyone. Women with a history of breast cancer, unexplained vaginal bleeding, previous blood clots, or high cardiovascular or stroke risk usually should avoid it, and stopping HRT may require follow up bone checks and a switch to another osteoporosis medication if fracture risk stays high.
Medications for Improving Bone Density
If osteoporosis is diagnosed or fracture risk is high, medication can be lifesaving for bone integrity. Major guidelines recommend:
- Bisphosphonates (first line therapy): These are the usual starting drugs for osteoporosis because they strongly reduce bone breakdown and lower spine and hip fracture risk. They’re taken weekly or monthly by mouth, or yearly by IV, and treatment is typically reviewed after 3 to 5 years.
- Denosumab (strong antiresorptive option): Denosumab is a 6-monthly injection that blocks a key bone-resorption pathway, leading to quick BMD improvement and fewer fractures. It must never be stopped suddenly, so a planned switch to another drug is needed to prevent rebound bone loss.
- Anabolic therapies (build new bone): These medicines actively stimulate new bone formation, so they’re used for women at very high fracture risk or with multiple fractures. Use is usually limited to about 2 years, then followed by an antiresorptive to keep the gains.
- Romosozumab (dual action therapy): Romosozumab both builds bone and slows breakdown, giving rapid BMD gains in high-risk postmenopausal women. It’s used for about 12 months only and then followed by long-term antiresorptive therapy to maintain results.
- SERMs (selective estrogen receptor modulators): SERMs act like estrogen on bones, helping preserve spine BMD and reduce vertebral fracture risk. They’re mainly an option for select postmenopausal women who need spine-focused protection and aren’t suited to other therapies.
Common Myths and Facts
Many women delay screening or treatment because of common misunderstandings about menopause and bone loss. Clearing up these myths helps you recognize risk earlier and take the right preventive steps before fractures happen.
| Myth | Fact |
| Bone loss after menopause is unavoidable. | Menopause speeds bone loss, but resistance training, weight bearing exercise, proper calcium and vitamin D, and treatment can slow it and sometimes improve BMD. |
| If I do not feel pain, my bones are fine. | Osteoporosis is usually silent; many women have no symptoms until a fragility fracture occurs. |
| Osteoporosis is only a problem for very old women. | The fastest bone loss often happens in the first 3 to 5 years after menopause, so risk rises in the 50s and 60s too. |
| Calcium and vitamin D supplements alone prevent fractures. | Nutrients help meet bone needs, but supplements alone do not reliably prevent fractures without exercise and overall risk management. |
| Walking is enough to build strong bones. | Walking supports bone, but resistance training gives the strongest stimulus for preserving or increasing BMD after menopause. |
| A fracture after 50 is just bad luck. | A low impact fracture after 50 suggests fragile bone and should trigger osteoporosis evaluation and prevention. |
Conclusion
After menopause, estrogen falls, bone loss speeds up, and osteoporosis risk rises, often silently until a fracture happens. Early DEXA screening is important, especially after 50 or with risk factors like early menopause, family history, low BMI, smoking, inactivity, alcohol use, or long-term steroids. Prevention includes calcium, vitamin D, protein, weight-bearing and resistance exercise, balance training, and healthy habits. If risk is high, hormone therapy or drugs like bisphosphonates, denosumab, SERMs, or anabolic agents can reduce fractures, alongside regular follow-ups and fall prevention.
FAQs
Does every woman develop osteoporosis after menopause?
No, not every woman will develop osteoporosis. Menopause increases risk because estrogen drops, but many women maintain strong bones with healthy lifestyle habits, good nutrition, and early screening. Managing risk factors early makes a big difference.
What are the first signs of bone loss after menopause?
In the early stages, there are usually no symptoms. Bone loss is often silent until a fragility fracture occurs. Subtle clues like slight height loss or back discomfort may appear later, but the most reliable early detection is a DEXA scan.
How often should postmenopausal women get a DEXA scan?
Most women should be screened at age 50 or soon after menopause, then every 1–2 years depending on results and risk level. Your doctor may suggest earlier or more frequent scans if you have strong risk factors.
How quickly does bone loss happen after menopause?
Bone loss is fastest during the first 3–5 years after menopause. After that, it continues more slowly but steadily, which is why early prevention and regular follow-up are important.
What are the main risk factors for postmenopausal osteoporosis?
Common risks include age over 50, early or surgical menopause, family history, low BMI, smoking, heavy alcohol use, inactivity, long-term steroid use, and medical conditions like thyroid disease, diabetes, rheumatoid arthritis, or malabsorption problems.
Can bone loss after menopause be reversed?
Lost bone is difficult to fully restore, but you can slow or stop further loss, and sometimes improve density with the right combination of exercise, nutrition, and medication if needed. Early action offers the best results.
How much calcium and vitamin D do I need after menopause?
Most guidelines recommend about 1,200 mg of calcium daily and 800–1,000 IU of vitamin D per day if diet or sunlight is insufficient. Food sources are preferred first, with supplements added only if needed.
What type of exercise is best for building bone strength?
Weight-bearing activities like walking, stair climbing, and dancing help maintain bone, but resistance training with weights or bodyweight is especially effective for protecting spine and hip density. Balance exercises also lower fall risk.
Is walking alone enough to prevent osteoporosis?
Walking is helpful, but on its own it may not be enough to preserve bone density in high-risk areas. Adding resistance training 2–3 times a week provides a stronger bone-building signal.
When is hormone replacement therapy used for bone health?
HRT is most useful for women in early postmenopause who also have symptoms like hot flashes. It helps reduce rapid bone loss, but it’s not appropriate for everyone, especially those with certain cancer, clotting, or cardiovascular risks.
What medications are used if osteoporosis is diagnosed?
Options include bisphosphonates, denosumab, SERMs, and anabolic bone-building drugs. These treatments either slow bone breakdown or stimulate new bone growth, helping reduce fracture risk.
What else besides bone strength prevents fractures?
Fall prevention is critical. Balance training, good vision care, safe home environments, supportive footwear, and managing medications that cause dizziness can greatly reduce fracture risk and help maintain independence.
References
- Dr Sarwinee Ratchanon. (2023, August 14). How does menopause increase the risk of osteoporosis? MedPark Hospital. Retrieved November 25, 2025, from https://www.medparkhospital.com/en-US/lifestyles/how-does-menopause-increase-the-risk-of-osteoporosis
- How does menopause affect bone loss in women? (2025, July 10). Impact. Retrieved November 25, 2025, from https://impact.deakin.edu.au/2025/07/how-does-menopause-affect-bone-loss-in-women/
- John Fernandez. (2025, June 26). Understanding Menopause and Bone Health: What Every Woman Should Know. Baptist Health. Retrieved November 25, 2025, from https://baptisthealth.net/baptist-health-news/understanding-menopause-and-bone-health
- Menopause and osteoporosis. (n.d.). Better Health Channel. Retrieved November 25, 2025, from https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/menopause-and-osteoporosis
Aubrey Carson is an RDN with 9 years across hospital, outpatient, and private practice settings. They earned an MS in Clinical Nutrition from Tufts University – Friedman School (2016) and completed a Dietetic Internship at Mayo Clinic. Aubrey specializes in micronutrient assessment, evidence-based supplementation, and patient education. Their work includes CE presentations for the Academy of Nutrition and Dietetics and collaborations with Mass General Brigham on nutrition education resources.

