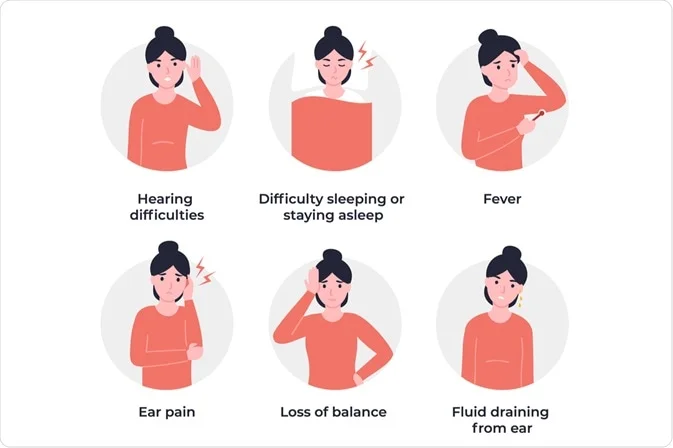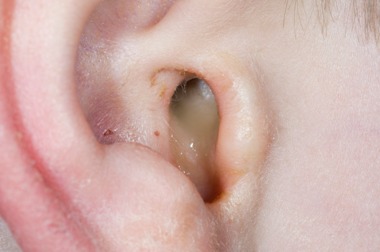
An ear infection occurs when bacteria or viruses inflame parts of the ear outer, middle, or inner causing pain, fluid buildup, or hearing loss. Understanding overall ear health is important for recognizing early risks. Signs and Symptoms of an Ear Infection vary by infection site, affecting hearing, balance, and comfort differently.
Key Takeaways
- Three types: outer (otitis externa), middle (otitis media), and inner (labyrinthitis) infections.
- The outer ear shows itching, pain when touched, and fluid discharge after swimming or cleaning.
- Middle ear infections cause sharp pain, fever, muffled hearing, and fluid buildup, often after colds.
- Inner ear issues affect balance, causing dizziness, nausea, or ringing in the ears.
- Infants show irritability, ear pulling, or poor feeding; adults feel pain or fullness.
- Red flags include severe dizziness, facial weakness, or swelling behind the ear needing urgent care.
What Is an Ear Infection
An ear infection happens when germs such as bacteria or viruses enter and inflame part of the ear. It can affect the outer ear canal, the middle ear behind the eardrum, or the inner ear, which controls balance and hearing. The symptoms depend on which part is infected and how severe it becomes.
Why Symptoms Depend on Location
Each section of the ear serves a different function. The outer ear collects sound, the middle ear amplifies it, and the inner ear processes sound and balance. Because of this, outer ear infections usually cause surface irritation, while middle or inner ear infections affect hearing and balance.
Signs and Symptoms of an Ear Infection
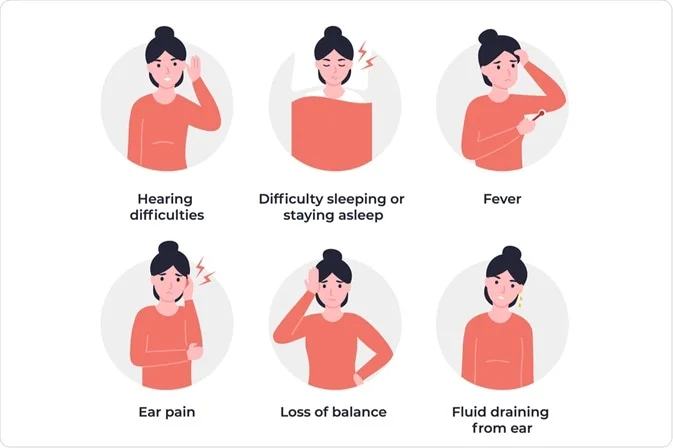
There are three main types of ear infections: the outer ear infection (otitis externa), the middle ear infection (otitis media), and the inner ear infection (labyrinthitis).
- Outer Ear (Otitis Externa)
Outer ear infection, often called swimmer’s ear, usually affects the ear canal skin. It can appear after swimming, cleaning, or scratching the ear.
Major Symptoms:
- Pain or tenderness, especially when pulling the outer ear
- Itching or irritation inside the ear canal
- Redness and swelling around the opening of the ear
- A feeling of fullness or blockage
- Fluid or discharge that may be clear, yellow, or thick
- Temporary hearing loss due to swelling or trapped debris
Typical Context
- Recent swimming, bathing, or exposure to water
- Cleaning too deeply with cotton buds or objects
- Hot, humid environments or skin conditions like eczema
What to Look For
- Pain increases when touching the ear flap or pressing the small bump in front of the canal
- Red, swollen ear canal
- Itching that turns painful or leads to drainage
- Middle Ear (Acute Otitis Media)
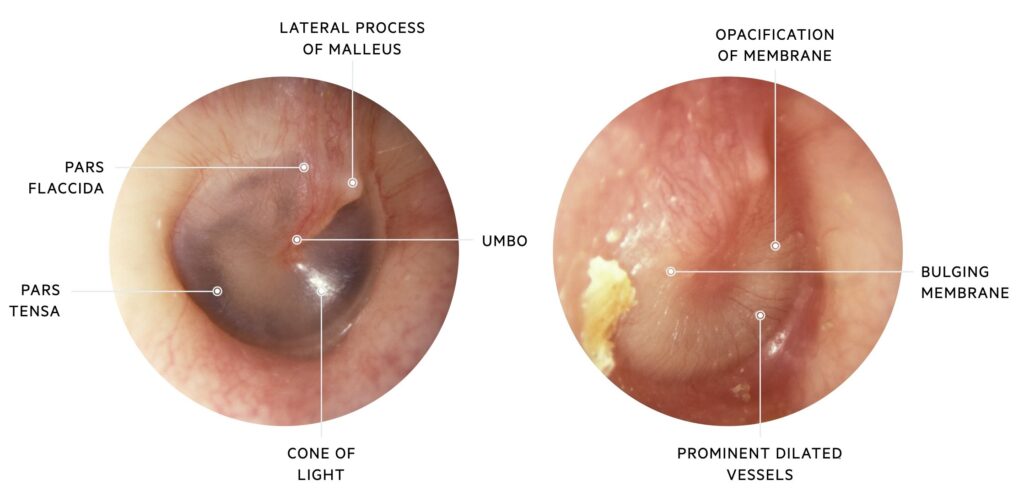
Middle ear infections are common in children but can also affect adults. They often start after a cold or sinus infection.
Major Symptoms
- Sharp or dull ear pain that may worsen at night
- Fever and irritability
- Hearing difficulty or a muffled sensation
- Trouble sleeping or feeding in young children
- Discharge if the eardrum bursts
- A sense of fullness or pressure inside the ear
Typical Context
- Often follows a cold, sore throat, or nasal congestion conditions that can also be associated with hearing loss if prolonged.
- More frequent in children because their ear tubes are shorter and drain less effectively
What to Look For
- Pain that suddenly improves followed by fluid or pus
- Crying or tugging at the ear in toddlers
- Loss of hearing or imbalance during recovery
Inner Ear or Balance Involvement Key Symptoms
When the infection spreads deeper, the inner ear or balance system may become affected.
Major Symptoms
- Sudden spinning or dizziness
- Nausea or vomiting that worsens with movement
- Loss of balance or coordination
- Ringing or buzzing sound in the ear
- Temporary hearing loss
Typical Context
- May appear after untreated middle ear infections
- Can also occur after viral illnesses affecting the nerves of the inner ear
What to Look For
- Spinning sensation even when still
- Unsteady walking or difficulty focusing
- Nausea combined with ear pain or hearing change
What You Can Feel or Notice (Self-Observed Symptoms)
These are the subjective signs of things that you personally experience or notice without any special tools.
- Pain or Discomfort: Often the first sign. The pain may be sharp, dull, or throbbing. It can worsen when lying down or chewing.
- Itching: Common in outer ear infections (otitis externa). It can feel like irritation or tickling inside the ear.
- Discharge or Fluid Leakage: You might notice clear, yellow, or pus-like fluid coming out of the ear. This often indicates an infection or a ruptured eardrum.
- Reduced Hearing or Fullness: Sounds may seem muffled, or the ear might feel “blocked” due to fluid buildup or swelling.
- Children’s Behavioral Signs: Since children can’t always express ear pain, you may notice crying more than usual, trouble sleeping, refusal to feed, pulling or rubbing their ears, or increased irritability.
What a Clinician Observes (Medical Examination Findings)
These are objective findings that a doctor can see or detect using specialized instruments like an otoscope.
- Red or Bulging Eardrum: Indicates inflammation or infection behind the eardrum (middle ear infection). The bulging shows pressure from trapped fluid or pus.
- Fluid or Air Bubbles Behind the Eardrum: Seen through the otoscope, these suggest the presence of fluid in the middle ear is a sign of infection or poor drainage.
- Swelling and Redness in the Ear Canal: Common in outer ear infections. The canal may look inflamed, narrowed, or even have visible discharge.
- Eardrum Movement (Reduced or Absent): Using a device that blows a small puff of air, a clinician checks eardrum flexibility. A stiff eardrum suggests fluid buildup behind it.
- Temperature and General Check: The doctor may also note fever or general illness signs that support an infection diagnosis.
Infants and Toddlers (Under 3 years)
At this age, children cannot clearly express what they feel, so parents need to watch for behavioral and physical clues.
- Crying and Irritability: Infants may cry more often, especially when lying down, because pressure in the middle ear increases in that position.
- Ear Pulling or Tugging: Babies might frequently touch or pull their ears due to discomfort or pain, though this can also happen from teething so it’s important to note other symptoms too.
- Poor Feeding: Sucking and swallowing increase ear pressure, which can make feeding painful. As a result, babies may refuse to feed or eat less.
- Restless Sleep: Lying flat increases ear pressure, causing pain that can wake the child frequently.
- Fever Without a Clear Source: Sometimes the only sign of an ear infection in very young children is a fever, even when there are no visible ear symptoms.
Why it matters: Early detection prevents complications like prolonged infection or hearing delays that can affect speech development.
Preschool and School-Age Children (3–12 years)
Children in this group can usually describe what they feel, making diagnosis easier.
- Complaints of Ear Pain or Blocked Ears: They may say their ear “hurts” or “feels full.” This often points to middle ear infection (otitis media).
- Hearing Difficulty: Fluid buildup can temporarily reduce hearing, making children seem inattentive or less responsive. Teachers may notice they don’t follow instructions well or ask for repetition.
- Ear Discharge (Fluid Leakage): If the eardrum ruptures, you might see clear, cloudy, or pus-like drainage from the ear canal.
- Trouble Paying Attention or School Difficulties: Reduced hearing can affect speech clarity, learning, and classroom focus.
Why it matters: Recognizing these symptoms ensures treatment before hearing or learning are impacted.
Adolescents and Adults
Older individuals are more likely to develop outer ear infections (otitis externa) rather than middle ear infections.
- Sharp or Sudden Pain: Pain may occur after swimming (“swimmer’s ear”) or after showering, when moisture remains trapped in the ear canal.
- Itching and Fullness: Persistent itching or a blocked sensation inside the ear canal is common as the lining becomes inflamed.
- Tenderness When Touching the Ear: The outer ear and area around it may be painful to touch, unlike middle ear infections where the pain is deeper.
- Possible Discharge: Fluid or pus may drain from the canal if the infection worsens.
Why it matters: Prompt treatment prevents chronic irritation and hearing issues, especially in those frequently exposed to water or who use earbuds often.
Symptom Timeline for Middle Ear Infection
The course of infection often follows a pattern.
1. Early Stage (Onset Phase)
This is when the infection begins to develop, often following a cold, sore throat, or nasal congestion.
How it starts:
The infection usually begins when the Eustachian tube (which connects the middle ear to the back of the throat) becomes blocked due to mucus or swelling from an upper respiratory infection or allergies.
Symptoms you may feel:
- Mild pressure or fullness in the ear
- Dull discomfort rather than sharp pain
- Muffled hearing or a sensation as if the ear is “plugged”
- No or low fever at this stage
Why it matters: This is the best time for early medical evaluation. If treated or monitored promptly, the infection may not progress further.
2. Acute Stage (Peak of Infection)
At this point, the infection is fully active, and inflammation and fluid buildup in the middle ear cause more noticeable symptoms.
What’s happening inside the ear: The trapped fluid becomes infected with bacteria or viruses, increasing pressure behind the eardrum. The eardrum may become swollen, red, and bulging.
Symptoms you may notice:
- Severe ear pain, often continuous or throbbing
- Fever (especially in children)
- Noticeable hearing loss or difficulty understanding speech
- Irritability, poor sleep, and appetite loss (especially in kids)
Clinical findings: Doctors often see a bulging, red eardrum and may detect fluid or pus behind it.
Why it matters: This is the most painful phase. Without treatment, pressure can increase enough to cause eardrum rupture.
3. Perforation or Relief Stage
If the pressure becomes too high, the eardrum may rupture (tear slightly), allowing pus or fluid to drain out of the ear.
What happens then:
- Pus or fluid drains from the ear canal this may look yellow or blood-tinged.
- The pain often decreases suddenly, because the pressure behind the eardrum is released.
Healing phase: The eardrum usually heals naturally within a few weeks, and hearing begins to gradually improve. Any remaining fluid may take days to clear completely.
Important note: While relief of pain feels like improvement, medical follow-up is essential to ensure full healing and prevent complications such as chronic ear infections or hearing problems.
Pain Patterns and What They Indicate
- Outer Ear Pain: Pain increases when the outer ear is touched or when the jaw moves. This suggests inflammation in the ear canal, often due to otitis externa (swimmer’s ear).
- Middle Ear Pain: Feels deeper, heavier, or pressured, often after a cold. It may be linked to otitis media, where fluid builds up behind the eardrum.
- Pain That Suddenly Disappears: If sharp pain fades and fluid drains out, this usually signals a ruptured eardrum, where pressure buildup caused a tear.
- Hearing and Balance Changes: The ear plays a key role in both hearing and maintaining body balance. When an ear infection develops, it can interfere with these two main functions: the ability to perceive sound clearly and to stay oriented or steady.
Ear Discharge and Its Meaning
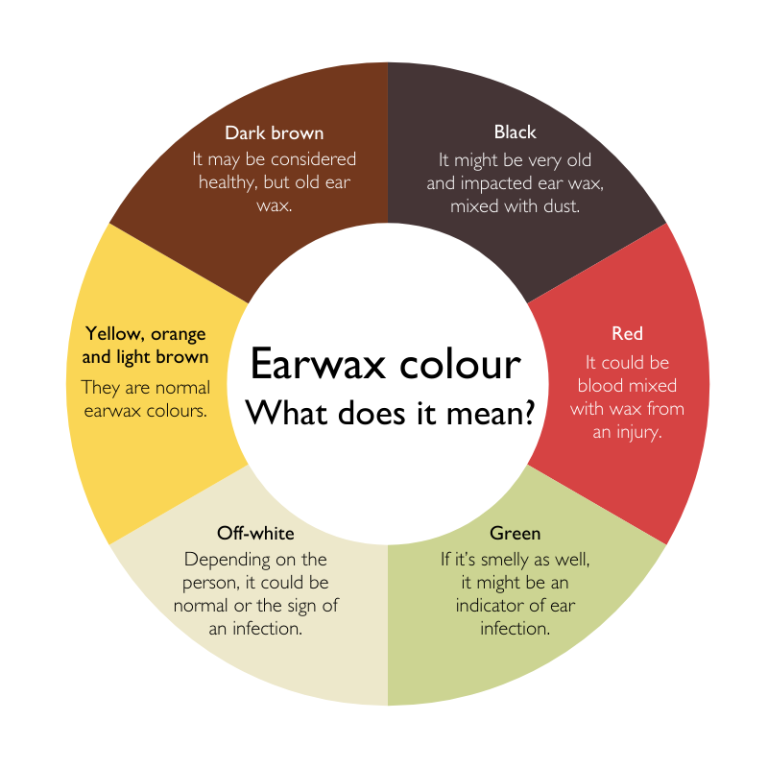
Discharge (otorrhea) provides diagnostic clues:
- Clear or thin fluid : mild irritation or allergy.
- Thick, yellow, or green discharge: bacterial infection.
- Foul odor: chronic infection or fungal cause.
- Sudden drainage after pain : possible eardrum rupture.
Systemic Symptoms and Related Conditions
Ear infections often come with whole-body symptoms, especially in children:
- Fever, fatigue, irritability, vomiting, or loss of appetite.
- Sore throat or nasal congestion from upper respiratory infection.
- Dry skin or eczema around the ear canal is common in chronic outer ear inflammation.
Red Flags Requiring Urgent Medical Care
Seek prompt medical attention for:
- Swelling, redness, or tenderness behind the ear.
- Ear protruding outward.
- Severe dizziness or sudden hearing loss.
- Persistent high fever or severe headache.
- Facial muscle weakness (possible nerve involvement).
- Stiff neck or confusion could suggest spreading infection (mastoiditis or meningitis).
Conditions That Mimic Ear Infections
Not all ear pain means infection. Other causes include:
- Earwax build-up or a foreign object.
- Jaw joint (TMJ) pain or dental problems.
- Pressure changes (flying, diving).
- Skin inflammation (eczema, allergic dermatitis).
it’s important to protect your ears to prevent worsening symptoms.
Risk Factors and Triggers
Common factors that increase ear infection risk:
- Swimming or frequent water exposure.
- Prolonged earbud or hearing aid use.
- Aggressive ear cleaning or inserting objects.
- Colds, allergies, or nasal blockage.
- Exposure to cigarette smoke.
Conclusion
Ear infections result from bacteria or viruses affecting the outer, middle, or inner ear. Outer ear infections cause itching, pain, and discharge, while middle ear infections bring fever, sharp pain, and hearing difficulty. Inner ear infections disrupt balance, causing dizziness and nausea. Children show irritability and ear pulling; adults may feel fullness or tenderness. Common triggers include swimming, ear cleaning, or colds. Seek urgent care for dizziness, facial weakness, or swelling. Early treatment prevents lasting hearing problems and relieves pain quickly.
FAQs
How can I tell an ear infection from a regular earache?
An infection often brings fever, discharge, or hearing changes, while a simple earache usually does not. Symptoms also tend to last longer and worsen without treatment. If the pain is increasing rather than improving, infection is more likely.
Does an itchy ear always mean infection?
No, it can result from dryness or irritation. Persistent itch with pain or discharge may mean infection. If itching interferes with sleep or daily activities, it’s worth getting checked.
Can you have an ear infection without fever?
Yes. Many outer ear infections and mild cases occur without fever. Other signs like pain when touching the ear or ear canal swelling can still be present.
What does smelly discharge mean?
It often suggests bacterial or long-standing infection that needs treatment. A foul odor usually indicates trapped moisture or debris in the ear. Prompt evaluation helps prevent complications.
Why did the pain stop but fluid appeared?
The eardrum may have burst, releasing fluid and easing pressure. This often brings quick pain relief but still requires medical care. The eardrum typically heals, but it should be monitored.
When should I go to the hospital?
If you have swelling behind the ear, severe dizziness, hearing loss, or persistent high fever. These may signal a spreading infection or mastoid involvement. Urgent assessment ensures timely treatment.
Can flying or diving cause similar symptoms?
Yes, pressure changes can cause temporary pain or blockage without infection. This is called barotrauma and often improves with equalizing techniques. If symptoms persist after travel, an exam is recommended.
Why are ear infections more common in children?
Children’s ear tubes are shorter and flatter, making it easier for germs to enter and fluid to stay trapped. Their immune systems are also still developing. This combination increases infection risk.
Can ear-buds or hearing aids cause infection?
If not cleaned properly, they can trap moisture and bacteria, leading to irritation or infection. Regular cleaning and drying helps prevent problems. Make sure devices fit comfortably to reduce friction.
Can an ear infection cause permanent hearing loss?
Most infections heal completely, but repeated or untreated infections can cause lasting damage. Scarring or chronic fluid buildup can affect hearing over time. Early treatment lowers these risks.
Reference
- Centers for Disease Control and Prevention (CDC) – Ear Infections
https://www.cdc.gov/antibiotic-use/ear-infection.html - Cleveland Clinic – Ear Infections: Causes, Symptoms & Treatment
https://my.clevelandclinic.org/health/diseases/8627-ear-infections - Johns Hopkins Medicine – Otitis Media (Middle Ear Infection)
https://www.hopkinsmedicine.org/health/conditions-and-diseases/otitis-media-middle-ear-infection - National Institute on Deafness and Other Communication Disorders (NIDCD) – Ear Infections in Children
https://www.nidcd.nih.gov/health/ear-infections-children - WebMD – Ear Infection Overview
https://www.webmd.com/cold-and-flu/ear-infection/default.htm
Autum Harkins is a CNS with an MS in Clinical Nutrition from Maryland University of Integrative Health (2017) and 8 years in integrative clinics. She develops individualized protocols for deficiencies, digestive health, and women’s wellness, prioritizing third-party-tested supplements. Autum contributes to case series and webinars and mentors practitioners on lab interpretation. Credentials: CNS Board (ANA/BCNS) number, state nutrition licensure where applicable, and professional memberships with links.